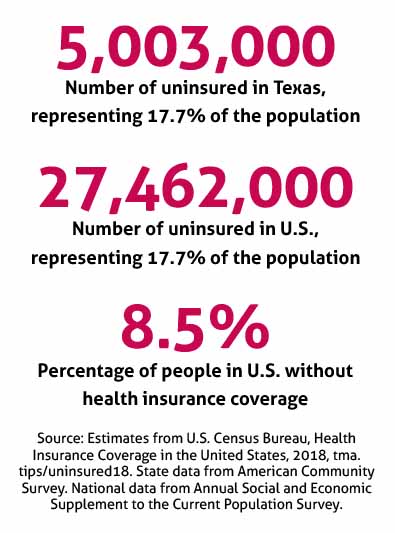
When you hear that more than 5 million Texans – more than one-sixth of the state’s population – are uninsured, your first reaction might be sympathy. You might think it’s a terrible thing for the people and families who fall in that category who can’t afford or don’t qualify for coverage. Maybe you’ll feel sadness as both a physician and a person.
And maybe your thought process just stops there.
But the impact of having the highest uninsured rate in the nation doesn’t. Sogol Pahlavan, MD, knows.
“I want people to understand, it’s not [happening in] a vacuum,” said Dr. Pahlavan, chief operating officer and managing partner at ABC Pediatric Clinic, located in a low-income community in east Houston.
Data compiled by the Texas Medical Association and other organizations, as well as physicians’ own anecdotal experiences, show how 5 million uninsured patients in Texas become 5 million dominoes. As they fall, so do countless others representing the health of Texas: The economy and well-being of entire communities. The classmates and friends of uninsured children. And yes, the physicians who deal with the burdens of treating uninsured patients in emergency rooms and providing uncompensated care.
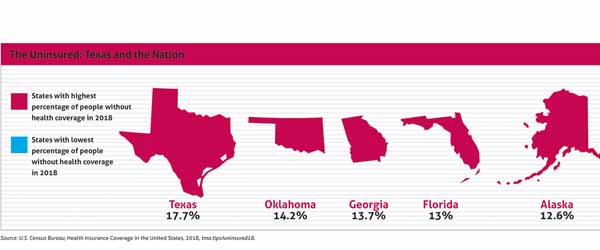
That’s all part of what makes Texas’ uninsured percentage last year – the nation’s worst at 17.7%, according to the most recent U.S. Census Bureau statistics – so troubling for medicine. TMA continues to stress to state lawmakers the gravity of having millions of uninsured residents, and to push constructive solutions the government must take to help.
The domino effect
The 2018 census numbers, released in September 2019, showed Texas’s uninsured population growing for the second consecutive year. Only Texas topped the 5-million-uninsured mark, and no other state had even 15% of its population uninsured in 2018; Oklahoma was second-worst at 14.2%. (See “The Uninsured: Texas and the Nation,” below.)
Dr. Pahlavan knows how the dominoes fall because she sees the population that often loses coverage and finds its way into the uninsured pool: Medicaid recipients. Texas was one of 14 states that didn’t expand Medicaid under the Affordable Care Act.
About 70% of Dr. Pahlavan’s patients are enrolled in Medicaid. Within the past year, she said, the clinic had seen about a 5% drop in its Medicaid patients, and a corresponding 5% increase in its share of uninsured, self-pay patients.
Because of financial constraints, Dr. Pahlavan says, only a minority of those uninsured patients are still getting their annual well-child checks. And lack of coverage creates countless problems, she says. When children are uninsured and their parents can’t afford their asthma inhalers, for example, children will get much sicker when viral infections or flu are in the air – leading to more hospitalizations and emergency department visits. The cheapest ADHD medication is also expensive for low-income parents, Dr. Pahlavan adds. And when children can’t take their prescribed ADHD medication, it affects not only their academic success, social success, and confidence, she says; it also affects the other students in the classroom.
And the impact doesn’t stop there.
“Ultimately, it’s going to affect the entire community, because [if] you don’t support a child in their academic and mental health, that’s going to further deteriorate,” Dr. Pahlavan said. “They’re going to have self-confidence issues. They’re going to get frustrated, angry, and bitter. This feeling of despair will in turn lead to anxiety, depression, and [ultimately] suicide. This is kind of the [trend] that we see in these kids as they age into the middle school and the high school years.”
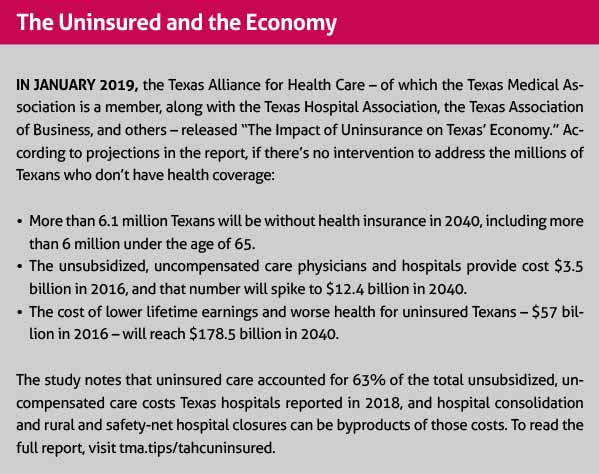
A recent study by the Texas Alliance for Health Care reveals the ripple effects of uninsurance throughout the Texas economy. (See “The Uninsured and the Economy,” page 28.)

New Braunfels family physician Emily Briggs, MD, routinely encounters the stories that have pushed the state past the 5 million uninsured mark.
“I regularly hear that my patients’ family members, if it’s not my patients themselves, [lost their] insurance because of a job change, or because they had Medicaid for pregnancy and then fell off of that and didn’t qualify for something else,” she said.
Dr. Briggs regularly sees the perpetual problem of uninsured patients using the emergency department for their primary care.
“By the time they’re able to obtain care, the [health] issue is already way beyond where it needs to be. Or, they have an issue that is very minor, but they don’t have access otherwise, so they end up going to the emergency department to obtain care for an upper respiratory infection.”
The Texas Alliance for Health Care report noted that children with health insurance, similar to adult employees who are insured, “have fewer school absences than the uninsured because they receive more preventive care, such as flu shots, and have improved overall health.” Students with healthy parents are less likely to miss school, the report said.
It also cited numbers showing that U.S. workers miss 407 million days of work annually – and those who go to work sick, and can’t concentrate as a result, negatively impact 478 million days of work. When workers are at work but are less productive because of poor health, it’s known as “presenteeism.”
It concerns the state’s business community enough to track that aspect of the problem.
“We certainly want to ensure that there’s a flexibility for business owners to be able to find those avenues to continue providing health care,” said Jessica Boston, manager of government affairs for the Texas Association of Business. “But with costs continuing to accelerate even for employers, certainly our small businesses specifically are having to make that choice of if they can even provide health insurance to their employees.”
The importance of funding
Physicians also stress the importance of funding primary care and preventive care.
Edinburg internist Linda Villarreal, MD, chair of TMA’s Board of Trustees, practices in Hidalgo County, historically the Texas county with the highest uninsured percentage. She says south Texas contains a large number of adults ages 18 to 24.
“Those are the people that are actually either in school or getting out of school and starting to work or starting a family, and they can’t afford insurance,” she said. “The only thing they’re going to get is if they have children, or if [a] woman is pregnant, they might be eligible for Medicaid insurance. But because it is so underfunded, access is very limited. And the payment to physicians has not really increased significantly in the last umpteen years. So the access to a physician who’s willing to take new Medicaid patients is also quite limited.”
She adds that “as much as we hate to talk about money, that is one of the biggest problems in making improvements in our uninsured population down here,” because the uninsured in her area are largely the working middle class who can’t afford private insurance. Better coverage would lead to good results, she says.
“If we could get better insurance coverage for our population, we could do wellness, we could do prevention. That means healthy kids,” Dr. Villarreal said. “Healthy kids get to go to school. Parents get to go to work. It’s kind of like a sequela of positive things.”
Along with higher physician Medicaid payments, TMA also pushed for Medicaid managed care reform during the 2019 legislative session. Lawmakers did follow through on some reforms, including measures that give patients more transparency on prior authorization denials and greater opportunity to challenge those denials.
But there’s much more work facing medicine in the year to come.
During the Texas Legislature’s “off” year in 2020, the Senate Business and Commerce Committee will study ways to decrease the uninsured rate. Medicine’s best route to making progress still lies in “Advocacy, advocacy, advocacy, with a capital ‘A’,” said Dr. Villarreal.
Tex Med. 2019;115(12):26-28
December 2019 Texas Medicine Contents
Texas Medicine Main Page