
Like many public health problems, obesity has become difficult to address in part because people consider it normal or even unavoidable, says Stephen Pont, MD, medical director of the Office of Science and Population Health and acting state epidemiologist at the Texas Department of State Health Services.
“People can become used to their situation,” he said. “And some folks can forget how they’re feeling and self-perceive that they’re feeling OK. They’ve forgotten how good they can feel [without obesity.]”
That circumstance can have deadly consequences, says Dr. Pont, who directed a childhood obesity center and was the founding chair of the American Academy of Pediatrics section on obesity. Years ago, he treated a 19-year-old man with severe obesity in another state who appeared at an emergency department one day with difficulty breathing. The man died within a week – almost certainly due to long-term, untreated comorbidities, such as sleep apnea and heart disease caused by his obesity, Dr. Pont says.
“He had just finished his first semester of college and was a straight-A student, so he had a very bright future ahead of him,” Dr. Pont says. “But [sleep apnea] really scares me because it can do a lot of damage without you realizing it’s happening.”

In fact, all types of obesity-related illnesses can do that kind of damage, says Lois Ramondetta, MD, a gynecological oncologist at The University of Texas MD Anderson Cancer Center in Houston and a member of the Texas Medical Association Council on Science and Public Health. Obesity causes or contributes to a range of fatal and debilitating health conditions, including heart disease, gall bladder disease, stroke, and diabetes. Higher amounts of body fat also are associated with increased risk of several cancers, including breast, endometrial, ovarian, thyroid, kidney, pancreatic, and colorectal cancers.
On top of this, obesity has emerged as one of the largest contributing factors in severe illness and death among those who contract COVID-19, according to several studies.
The U.S. Centers for Disease Control and Prevention (CDC) calls obesity an epidemic. In Texas, for instance, the rate of adult obesity soared from 10.7% in 1990 to 34.8% in 2018, according to data from the Robert Wood Johnson Foundation.
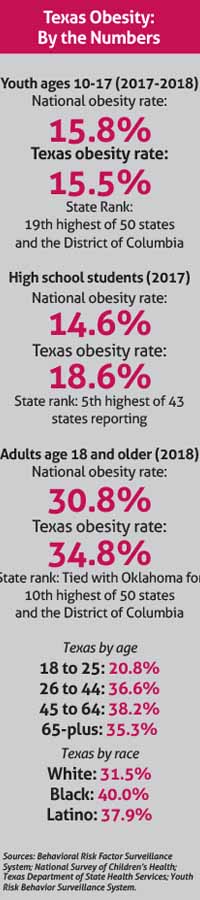
“Texas is typically in the top five to 10 states with the highest rates of obesity,” Dr. Pont said. (See “Texas Obesity: By the Numbers,” right.)
 Not only does being overweight and having obesity affect health and quality of life, it also can be a “minefield topic” for physicians, Dr. Ramondetta says. The public discussion on obesity often swings between emotional extremes, with some cruelly “fat shaming” those who are overweight or obese and others defending obesity as a lifestyle choice.
Not only does being overweight and having obesity affect health and quality of life, it also can be a “minefield topic” for physicians, Dr. Ramondetta says. The public discussion on obesity often swings between emotional extremes, with some cruelly “fat shaming” those who are overweight or obese and others defending obesity as a lifestyle choice.
Moreover, obesity is a complicated topic that touches on subjects ranging from psychology to genetics to poverty, says Eduardo Sanchez, MD, chief medical officer for prevention and chief of the Center for Health Metrics and Evaluation for the American Heart Association in Dallas.
The easiest way to prevent obesity is by educating the public – especially young people – about healthy foods and exercise, Dr. Sanchez says. But physicians also can learn to communicate more effectively. The best place to start is by understanding what obesity is.
“Obesity is a disease, and we don’t blame people for their disease,” he said. “Try to avoid even thinking that people are at fault for having obesity, as opposed to being obese.”
Complex causes
Obesity costs the U.S. about $150 billion a year in health care costs, or about 10% of all medical costs, according to CDC. Nationally, 1 in 3 adults and 1 in 6 children are obese, the agency says.
The problem is so severe it affects military recruiting. A 2018 study found one-third of 17- to 24-year-olds are too overweight to qualify for military service – the largest single reason for military disqualification (tma.tips/UnhealthyUnprepared).
Weight gain is caused by a person regularly consuming more calories than he or she can burn, which can lead to obesity. But obesity is caused by a complex interplay of factors, according to CDC. Those factors include:
• Behavior, especially as it relates to diet and exercise;
• Community environment, such as a neighborhood where a person feels safe to walk or bicycle, or a workplace that encourages healthy eating;
• Genetics, which in most cases involve a still poorly understood interaction between genes and a person’s environment;
• Family history, which affects genetics and upbringing as well as eating habits and exercise habits. (See “Obesity and Adverse Childhood Experiences,” above.);
• Diseases, which in rare cases such as Cushing’s disease can cause obesity; and
• Prescription drugs, such as steroids, which can cause obesity.
The obesity epidemic touches all demographic categories, Dr. Pont says. “Every group in America pretty much is challenged by its weight right now.”
However, obesity does not touch them all equally, Dr. Sanchez says. African Americans, Latinos, and Native Americans have a higher prevalence of obesity than do whites and Asians, and the reasons can be traced back in large part to social determinants of health – the conditions under which people live.
For instance, African Americans, Latinos, and Native Americans tend to have higher poverty rates, lower incomes, and lower education levels, all of which tend to contribute to less healthy eating habits.
All three groups also are less likely to have health insurance, Dr. Sanchez says.
“It’s not that not having insurance makes you obese,” he said. “It’s that not having insurance results in you not seeing a doctor and getting the screening, counseling, and referral that can make a difference.”
The American Medical Association first classified obesity as a disease in 2013. Since that reclassification and the passage of the Affordable Care Act, insurance plans have improved coverage for weight-related medical visits, according to the National Conference of State Legislatures.
However, the coverage is uneven. For instance, Texas Medicaid pays for bariatric surgery but not nutrition counseling or pharmacotherapy, according to a 2018 study in the journal Obesity (tma.tips/MedicaidObesity).
Responding to the epidemic
Physicians should respond to the obesity epidemic in two ways: by counseling patients and by supporting changes that make it easier for everyone to make healthy choices, Dr. Pont says.
Speaking with patients about obesity might seem obvious, but physicians concerned about keeping patient satisfaction scores high have an incentive to avoid topics that might anger patients, like obesity or end-of-life care, Dr. Ramondetta says.
“Let’s say you have 15 minutes to talk to a patient and you want to do the best for them,” Dr. Ramondetta says. “There may be [physicians] who shy away from difficult topics in order to continue with patient satisfaction. And talking about obesity [can be] a very difficult topic.”
Physicians and health care professionals who do speak to patients about obesity frequently take the wrong approach, Dr. Pont says.
“Unfortunately, health care providers are some of the worst offenders when it comes to weight stigma and bias,” he said. “Where that comes from is that we’re passionate about health and the health of our patient. We become frustrated and many of us shift to guilt and blame rather than using more strategic and effective motivational interviewing.”
Motivational interviewing is a counseling technique that helps patients get past insecurities, uncertainty, and ambivalence to find internal motivation that helps them change their behavior. However, most physicians have not been trained how to use the tool, Dr. Ramondetta says. (See “Motivational Interviewing,” page 40.)

“I talk to my patients about [obesity] on a regular basis, and yet I probably don’t do it in the most effective way,” she says. “My interest in doing motivational interviewing has increased, and I think it’s something that needs to be taught even at the medical school level.”
Working with patients to overcome obesity can be as multi-faceted as the disease itself, Dr. Sanchez says. Patients not only need better education about nutrition and physical fitness, they also need help breaking down barriers to those goals, such as finding healthier food options and more parks or walkable spaces.
Physicians also can engage in advocacy to address the societal factors that promote obesity, especially those that influence young people, Dr. Sanchez says. That includes making sure kids get healthy meals in schools and getting employers to improve food options for their employees.
“It’s not a one-size fits all [problem],” he said. “It doesn’t lend itself to writing a prescription and watching the medication take hold. It involves understanding each individual patient and the context in which that patient lives.”
Tex Med. 2020;116(7):38-41
July 2020 Texas Medicine Contents
Texas Medicine Main Page