
Texas’ rate of maternal deaths is slightly above the national level, long-awaited new data from the National Center for Health Statistics (NCHS) shows.
Texas’ maternal mortality rate of 18.5 per 100,000 live births in 2018 was just slightly above the newly revised U.S. rate of 17.4 per 100,000, according to data released today by NCHS, a branch of the U.S. Centers for Disease Control and Prevention (CDC).
The NCHS information is the first national estimate of maternal deaths since 2007. The new rate is based on a checkbox on death certificates, adopted gradually by the states since 2003, that helps identify deaths related to pregnancy.
In all, 70 women in Texas and 658 women nationwide died while pregnant or within 42 days of the end of pregnancy in 2018, the report says.
The NCHS data are an important step forward in understanding the problems that cause women to die during pregnancy, in childbirth, or shortly after, says Houston obstetrician-gynecologist Carla Ortique, MD, vice chair of the Texas Maternal Mortality and Morbidity Review Committee.
“In addition to being the first such release since 2007, it maintains focus on the unacceptable rate of maternal death in our state and country," said Dr. Ortique, who also is a member of the Texas Medical Association Council on Science and Public Health and a consultant to the Committee on Reproductive, Women’s, and Perinatal Health.
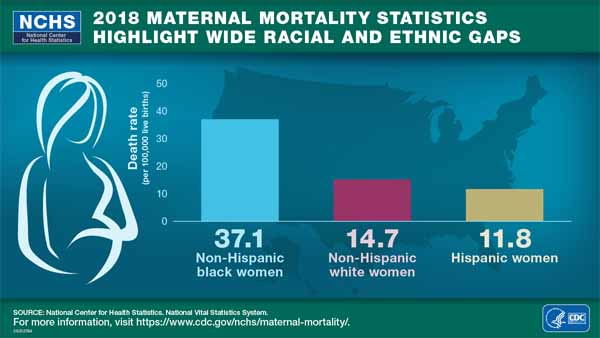
The NCHS report showed big disparities in the rates among racial and ethnic groups. The rate for non-Hispanic black women of 37.1 deaths per 100,000 live births was much higher than the rate for non-Hispanic white (14.7) and Hispanic (11.8) women. Those rates reflect trends found in Texas data on maternal deaths.
The U.S. rate is high compared with most other wealthy, industrialized countries. For instance, Canada’s 2018 maternal death rate was 8.3 deaths per 100,000 live births, according to Statistics Canada, the country’s national statistics office.
While the NCHS data are a big step forward in quantifying the problem, U.S. and state agencies are still refining ways to make it more accurate and uniform, says Dr. Ortique.
The NCHS report acknowledged this problem as well. It stated that “some of the variation in state rates is due to the differences in the quality of state maternal mortality data.”
Variation in the quality of reporting maternal deaths may be due to differences in electronic death registration systems and differences in policies and programs designed to verify the pregnancy status of females of reproductive age who die, the report said.
“Challenges continue to exist in identifying contributing factors and preventability of maternal death,” Dr. Ortique said. “Continued focus on improving data collection and standardization of the maternal death review process is essential to develop recommendations for the systems level changes necessary to eliminate both preventable maternal deaths and the racial, ethnic, and socioeconomic inequities that exist in the maternal death rate."
The Texas Department of State Health Services (DSHS) plans to release its own report on maternal deaths in late August, a spokesman told Texas Medicine in an email.
Texas’ death rate for all new moms was 14.6 per 100,000 live births in 2012, the last year for which there was accurate data. That was slightly below the national average of 15.9 per 100,000 for 2012, as reported by the CDC.
“We know that there are issues with maternal mortality data that rely solely on death certificates, as identified in our 2018 Obstetrics & Gynecology paper, and death certificate data alone will likely lead to an inflated maternal mortality rate,” the DSHS spokesman said. “That’s why we’re continuing to analyze the data through our enhanced method and plan to publish more years of results as part of the biennial DSHS/Maternal Mortality Review Committee Joint Report this summer.”
TMA has been working hard to stop all maternal deaths in Texas, including adopting an eight-point plan to protect the health of all pregnant women and new mothers.
A primary component of that plan: extending Medicaid coverage to 12 months for preventive, primary, behavioral, and specialty care before, during, and after pregnancy.
During the 2019 Texas legislative session, TMA strongly supported House Bill 744, which would’ve allowed continued Medicaid coverage for eligible women up to 12 months postpartum. HB 744 was voted out of the House 87-43, but did not get a hearing in the Senate.