
In the past two years, Match Day has brought unusual attention to emergency medicine: After four decades of steady popularity among medical students and physicians seeking residencies in that specialty, it turned in lower-than-expected performances both times amid an otherwise solid Match year.
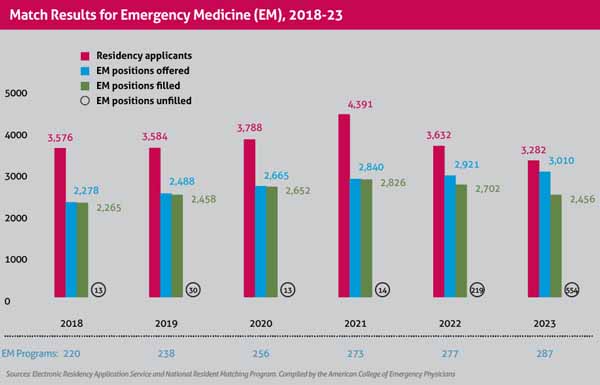
In 2023, emergency medicine offered 3,010 positions for medical students and physicians to fill, but 554 of them went unclaimed on Match Day – a fill rate of 81.6% compared with the overall match rate of 93.3%, in line with recent years. In 2022, 219 out of 2,921 emergency medicine positions remained unfilled after the initial match – a fill rate of 92.5% – which, at that time, was the highest number of unfilled positions the specialty had ever seen.
“Emergency medicine has always matched [at or near] 100% ever since it became a specialty,” said former Texas Medical Association President Diana Fite, MD, a Houston emergency medicine physician. “It’s been very popular among the smartest of the medical students, probably because it involves so much that is a challenge. You have to know something about everything, and you can make a difference in people’s lives.”
In both years, about 90% of the unfilled positions were quickly snatched up in the Supplemental Offer and Acceptance Program (SOAP) for unmatched medical students and physicians, says Woodson “Scott” Jones, MD, vice dean of graduate medical education for the UT Health San Antonio Long School of Medicine.
“A 90% fill-rate in the SOAP with so many positions available shows an ongoing strong degree of interest in the field,” he said.
Nevertheless, the sudden spike in unfilled positions on Match Day has been jarring for physicians in a specialty that fills its residency spots routinely.
The 2023 spike in unclaimed residency spots prompted 11 emergency medical organizations – including the American College of Emergency Physicians (ACEP) and the American Academy of Emergency Medicine – to form a task force to study the problem.
“The task force is working to identify factors that have led to an increase in unfilled [emergency medicine] positions and to develop strategies to mitigate them,” the coalition announced in a press release.
The factors it will study include workforce projections, increased clinical demands, emergency department (ED) overcrowding, economic challenges, the impact of the COVID-19 pandemic, and the corporatization of medicine, the release said.
Emergency medicine may need to make changes in its residency programs – especially in how many there are – but its recent Match experience has plenty of precedents, says San Antonio emergency physician Gillian Schmitz, MD, immediate past president of ACEP.
For instance, anesthesia went through a similar problem in the 1990s, she says. Concerns about workforce projections with managed care prompted speculation about a surplus of anesthesiologists, which affected perceptions of the specialty among medical students.
“They had a rapid decrease in the number of people applying to anesthesia, and they had a number of residencies that didn’t fill during that period,” Dr. Schmitz said. “They had about six years [of that] before it turned around. But workforce projections change over time as market conditions impact supply and demand, and forecasted predictions do not always turn out to be accurate. Today, you couldn’t hire an anesthesiologist if you tried, they’re in such high demand.”
Residents and future medical students may bear the brunt of restoring equilibrium to emergency medicine if the number of programs and positions goes down to correct the oversupply, as many expect, says Austin emergency physician Robert Emmick, MD, chair of TMA’s Committee on Physician Distribution and Health Care Access. Also, the disparity between supply and demand among residencies may persist for a while, creating more uncomfortable Match Days.
“Are people worried? Yes,” he said. “Is it going to work itself out? Yes.”
Much of the attention for the problem has focused on the news that fewer medical graduates are applying for emergency medicine residencies. There’s been a 26% decrease in the number of applications to emergency medicine residencies since 2021, according to data from the National Resident Matching Program, which runs the Match. This number is now widely viewed as indicating a decline in interest in emergency medicine by medical students.
But Dr. Schmitz disputes that fact as misleading because, she says, the pandemic year of 2021 was an outlier and not representative of a typical Match for emergency medicine. In the 2020-21 application cycle, emergency physicians were being hailed as health care heroes during COVID-19. Because of that, the specialty saw a record number of 4,391 applicants in 2021, which was unusual. The number of applicants in 2022 and 2023 are closer to the pre-pandemic baseline and only a slight decrease from where the specialty was pre-COVID.
“There has only been an 8% decrease in the number of emergency medicine applicants between 2023 and 2018,” she said.
More importantly, the main factor driving the surplus in residency spots for the past two Match Days is an increase in the supply of residency programs and residency positions, not a drop in interest from medical students, Dr. Schmitz says.
“The reason we have so many unmatched is primarily because of an explosion in the number of residency programs and now-available [first-year residency] slots, which are sort of diluting the competitiveness of the specialty,” she said. “Between 2014 and 2023, we had a 30% increase in the number of residency programs, a 46% increase in the number of [first-year residency] positions.”
This growth continued even after a December 2021 workforce study commissioned by ACEP showed that emergency medicine would likely face a nationwide emergency physician surplus of 7,845 by 2030.
That study was based on data from 2019, and the attrition rate post-pandemic is significantly higher than predicted, so the surplus is likely to be much lower, Dr. Schmitz says. But it still caused concern among students about careers in emergency medicine.
“That workforce study really shook the population of the specialty, with people fearing, ‘Am I going to have a job in five years?’” she said.
And it’s not just how many new positions are being created; it’s how they’re being created, Dr. Schmitz says. In the past, most residency programs were started by academic and nonprofit institutions. But the residency growth in programs is taking place among large corporate entities.
“We’re seeing a rapid increase in the number of for-profit hospitals and for-profit employers who are now starting residency programs,” she said.
Much of this can be attributed to the corporatization of medicine, Dr. Jones says. Many of these corporate-based hospitals are new or new to graduate medical education. So, when they start new residency programs, they may receive funding for the positions they create from the Centers for Medicare & Medicaid Services (CMS), not just for emergency medicine but for other specialties as well. Those corporate entities may be betting that they can save money over time by creating a kind of farm system for physicians, he says.
“It’s a logical thing to do because it grows your workforce and it brings in funding,” Dr. Jones said. “So, you’re paying less than you would to [physician assistants (PAs) and advanced practice registered nurses (APRNs)], and then you bring in CMS dollars, and you’re doing double well. And by the way, the graduates know your system, understand your workflow – they’re a real target for hiring.”
ACEP and other emergency physician groups have encouraged the Accreditation Council for Graduate Medical Education to scrutinize even more closely the standards for emergency medicine residency programs and identify programs that are not meeting them, Dr. Schmitz says.
“We’re hoping by increasing [scrutiny] and looking at the standards, that that will potentially decrease the number of programs,” she said. “But there’s also potentially likely to be some market forces. If we continue to increase the number of residency programs, and they don’t fill any of their spots for multiple years in a row, one would think that [the programs] would eventually close.”
The drop in applications for emergency medicine residency spots is concerning, Dr. Fite says. But every specialty has unique problems and stressors that can discourage medical students from looking at it as a career; emergency medicine is no different.
Some have been well-publicized – like the fallout from COVID-19, which hit emergency physicians particularly hard, she says. Burnout among U.S. emergency physicians rose from 47% to 60% from 2019 to 2021, according to the 2022 Medscape Physician Burnout & Depression Report.
“There is so much stress in emergency medicine … so it’s not surprising about the burnout,” Dr. Fite said.
Another factor in burnout and attrition is ED violence, Dr. Schmitz says. A 2022 ACEP survey found that 85% of emergency physicians believe the rate of violence experienced in EDs increased over the previous five years.
Burnout also is fueled, in part, by hospital finances, Dr. Fite says. In order to save money, hospitals increasingly require emergency physicians to see patients faster. At the same time, more patients in need of hospital care are being “boarded,” or left to wait – sometimes for days – in the ED until a hospital bed opens up, she says.
“You’ve got them lining the walls of the emergency department waiting for a bed,” she said.
Boarding is caused in part by demographic and societal problems, Dr. Schmitz says. The U.S. population is growing older and sicker, which means people need more emergency and hospital care. But in many cases, health care financing gives incentives to hospitals to operate at full capacity and prioritize elective surgeries – which make money – over people coming in through the ED, who are frequently poor and have no medical insurance.
“We’re competing against our own services for those hospital beds, and that puts a strain on the health care system that invariably backs up into the emergency department,” she said.
National shortages of emergency nurses add to this stress and frequently require physicians to practice “waiting room medicine” as EDs become overcrowded, Dr. Schmitz says. At the same time, there are constant scope-of-practice battles over the role of PAs and APRNs as hospitals look for ways to save money.
“Students have a lot of legitimate concerns about the future and hesitancy about picking a specialty based on a number of variables that are subject to change but are top of their mind right now,” Dr. Schmitz said.

Discouragement in emergency medicine could build on itself; however, those conditions are likely to change, Dr. Jones says. For instance, during the COVID-19 pandemic, medical students had less emergency medicine exposure because of safety concerns, limited personal protective equipment, and overwhelmed clinical services. But now they can get a better look at both the benefits and the drawbacks the specialty offers as a career.
“Students will have more opportunities to see fully functional and integrated teams,” he said. “There will be greater attraction to emergency medicine.”
And given what happened on the past two Match Days, emergency medicine residency programs are undoubtedly stepping up their recruitment of medical students, Dr. Jones says.
“They didn’t have to work [that hard to recruit] in the past,” he said. “That has passed. There will be more effort on the part of [emergency medicine] programs to recruit and woo into their field.”
Greater engagement and recruitment, along with a lower-than-expected surplus of emergency physicians and a strong history of interest by medical students, indicate that emergency medicine will make a strong recovery, Dr. Jones says. It’s just not clear how long that will take.
“Most of us feel this is going to balance out,” he said.