
Medical education in Texas faces many tough challenges, like shortages in clinical training space and getting enough students into high-need specialties like family medicine. But the 2025 session of the Texas Legislature showed that lawmakers still strongly support both residency programs and medical schools that can address these and other problems, says David Lakey, MD, chair of the Texas Medical Association’s Council on Medical Education.
“There’s a general recognition that we need to bring more physicians to Texas, grow more physicians in Texas, and expand that part of the workforce,” said Dr. Lakey, who is vice chancellor for health affairs and chief medical officer for The University of Texas System.
That growth is critical to keep up with Texas’ rising population – which leads the nation in numerical growth – and because the state has an aging general population and an aging population of physicians, says Marcia Collins, TMA’s associate vice president for medical education. While the 2025 session benefited both graduate medical education and undergraduate medical education, the most consequential news came in funding the expansion of residency programs because they lead directly to physician growth, Dr. Lakey said.
Graduate medical education (GME) is vital for building the physician workforce because numerous studies show that physicians typically set up medical practices near their residencies, he said.
“You’re at a time of your life as a physician when you’re making connections, starting a family, all those important things,” Dr. Lakey said. “That’s why it’s important to recruit [physicians] and bring them here to Texas during that time.”
One of the most important GME victories came in expansion grants, which are designed to strengthen and expand training opportunities. Before the 2025 session, the Texas Higher Education Coordinating Board (THECB) projected an additional $71 million (30.5%) would be needed for these grants in the 2026-27 biennium.
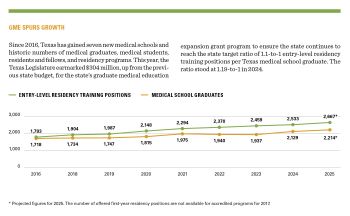
That amount was needed to support the residency positions created through the state’s expansion grant program since 2014 and also maintain the state’s target ratio of 1.1 entry-level residency position for every medical school graduate in the state, says Ms. Collins.
For instance, given the projected 2,350 Texas medical school graduates in 2026, it will take a 2,585 GME positions to maintain that target ratio of residents to graduates, Ms. Collins said. In 2027, there will be a projected 2,380 medical school graduates, requiring 2,618 GME positions to stay at 1.1 to 1.
Lawmakers came through with the $71 million for the expansion grants, raising the total funding to $304 million for the biennium. The expansion grants are prioritized for primary care and psychiatry.
In recent sessions, Texas lawmakers also have designated “mission-specific” funds that foster and promote each school’s strength. (See “Mission Driven,” page 8.)
These and other investments will bring in more physicians and improve medical education, says Thomas Mohr, DO, vice president for medical affairs and dean at Sam Houston State University College of Osteopathic Medicine (SHSU-COM). They also explain why medical educators in other states envy Texas physicians.
“I speak with people from medical schools in other states, and the Texas Legislature is bar none the best at funding medical education,” he said. “And the advocacy of the Texas Medical Association has gone into making that happen.”
Rep. Suleman Lalani, MD (D-Sugar Land), said via email to Texas Medicine that advocacy was decisive in turning a potentially “defensive session” into something positive because “physicians showed up in committee rooms, at First Tuesdays at the Capitol, and in thousands of messages and phone calls to lawmakers.” The result: a growing awareness among legislators about the problems faced by physicians and other health care professionals.
“Lawmakers understand if Texas does not train and keep enough physicians, every other health policy is just talking points,” he said. “The workforce investments we made this session reflect a growing consensus that medical education funding is one of the most cost-effective ways to improve access to care across the state.”
Lawmakers also prioritized support for the state’s 13 public medical schools. Those schools received $921 million for instruction and operations over two years, an 8.8% increase.
This included a first-time $11 million allocation for The University of Texas at Tyler School of Medicine, which started classes in 2023.
“That increase in instruction and operations funding gives our medical schools the stability to grow class sizes responsibly, invest in faculty, and expand clinical training sites, especially in high-need specialties,” Representative Lalani said.
In addition to the ongoing state funding to teach medical students, the University of Houston Tilman J. Fertitta Family College of Medicine also saw a spike in new funding from $20 million to $50 million designed to help the school, which opened in 2020, to expand class size, conduct research, hire additional faculty and staff, and support clinical operations. This 150% increase was one of the largest a Texas medical school received for this biennium.
The state has opened seven new medical schools – both public and private – since 2016, bringing the total to 16.
Several schools, including two that recently opened – UT Tyler and SHSU-COM – focus many of their resources on improving health care in rural areas, with SHSU-COM receiving $3.6 million in new mission-specific funding for a consortium for GME for rural and underserved areas.
“We have [health care] challenges across the state, but they are most pronounced in rural areas,” Dr. Lakey said.
With that in mind, lawmakers allocated $5 million to study the feasibility of setting up another medical school at Tarleton State University in Stephenville.
The study will be ready by the next legislative session in 2027, and – if the school receives legislative support and accreditation approval in Stephenville – it could help expose more medical students to the possibilities of setting up a practice in a rural area, said Adrian Billings, MD, member of the TMA Council on Legislation. Medical students studying in big cities – where most medical schools are located – seldom find rural practice attractive because they are used to big city amenities and the medical resources and technology found at large hospitals.
“The two biggest predictors of a future rural practitioner for a medical student are, one, having rural origin or some significant experience in a rural area, and, two, having exposure to rural medicine as a medical student and/or as a resident physician” – and preferably both, said the Alpine family physician, who is also chair of rural health with the F. Marie Hall Institute for Rural and Community Health at Texas Tech University Health Sciences Center School of Medicine.
Priming the rural pipeline
Lawmaker support for improving educational opportunities in rural medicine remained strong overall, Representative Lalani said.
The legislature doubled funding for the Texas A&M University Rural Engagement Program, to $30 million. This initiative, established in 2024, expands access to care in rural areas through the collaboration of physicians, nurses, and health care leaders at the Texas A&M University Naresh K. Vashisht College of Medicine. This program forges partnerships with rural communities, hospitals, clinics, and health care providers to broaden access and improve health care delivery.
Texas legislators also provided $5 million to THECB for the creation of a family medicine-obstetrics postgraduate training grant program, which is expected to improve access to care in rural areas with such shortages.
“[Family medicine] is the specialty of choice for rural physicians,” Dr. Billings said. “Although family medicine makes up only 9% of the physician workforce, family physicians account for 45% of the rural workforce. So, any investment in the family medicine residency program is likely to disproportionately and positively impact rural access to care.”
But there is plenty of unfinished business in addressing rural care, he said.
“What we need is multi-institutional rural health care training centers throughout our state that combine community colleges, four-year universities, and academic health centers to train health care students [in a multidisciplinary way] from the associate degree to the professional MD/DO degree at rural critical access hospitals,” Dr. Billings said. “These rural campuses can also be a place where rural-focused students can go to train rurally.”
Senate Bill 2695 authored by Sen. Lois Kolkhorst (R-Brenham), attempted to create such a pipeline into rural practice, he says. The bill, which TMA supported, passed the Senate but died in the House.
“Many of us would welcome that kind of innovative pipeline,” Representative Lalani said. “We are already investing in rural residency training and in stabilizing rural hospitals and telehealth, and a grow-your-own pathway from rural classrooms to rural clinics fits naturally with that strategy.”
Sean Price is a contributing editor and past associate editor for Texas Medicine.