Photo: Jake Margo, MD
There are inherent risks when caring for people who are sick with communicable diseases – risks that physicians take on as part of their duty and calling.
But COVID-19’s many unknowns – particularly early in the pandemic – along with the critical statewide shortages of personal protective equipment, elevated those risks even more.
So it’s no surprise that many physicians were among the more than 1.3 million confirmed COVID-19 cases in Texas last year. Despite taking numerous precautions to protect their patients, colleagues, family, friends, and communities, many physicians became sick, and unfortunately, some did not survive.
But as our understanding of the illness and our ability to treat it and defend ourselves against it have increased, the risks associated with caring for the sick have decreased.
Texas Medicine spoke with three Texas physicians who contracted COVID-19 to learn how the disease affected them physically and impacted their outlook as caregivers.
Ray Callas, MD, anesthesiologist, Beaumont
I was getting ready to go to the hospital one Friday morning in late July or early August, and I couldn’t bend down to tie my shoes – I was having severe back pain. I didn’t think anything of it because every morning I usually walk 2 to 3 miles and then lift some weights, so I just thought I had twisted something. I didn’t have any fever, didn’t have any cough, nothing like that; I just felt back pain. When I got off after working – I still wore [an N95 mask], all that stuff – I didn’t feel bad.
The next day my wife and friends were going to a restaurant, and it’s not like me not to go, but I just stayed home. By that time, not only my back hurt, but now it’s my legs and shoulders starting to hurt. I’ve never missed a day of work – ever – but I was supposed to work Monday, and I called a friend of mine Sunday and said, “If you wouldn’t mind working for me, I’m going to get a test.”
At that time, the only symptoms I had were severe pains all over my body. I went to a drive-through ER. They swabbed my nose, and came out about 30 minutes later to say, “Dr. Callas, I want you to know you have coronavirus.”
I quarantined myself into a room at home and laid in bed almost three days straight. But when it got scary was probably day five – isolation day two: My O2 stats were dropping into the low 90s. I didn’t want my oxygenation to go so low that I would need a breathing tube or become intubated, but thank God that never happened.
Even when we had H1N1, or even I’ve heard with HIV, we knew that we could protect ourselves by making sure we didn’t get stuck, or we didn’t have secretions get sprayed in our eyes. But this virus was so disrespected at first, and then it got real. And now I think people are over it, but they still respect it. This virus still causes people harm and even death. Like I tell everyone, I expect people to keep following what the data says – and what the scientific data says, not the biased opinion of others.
Carlos J. Cardenas, MD, gastroenterologist, Edinburg
My symptoms were relatively atypical in the beginning: It was primarily terrific myalgias and unrelenting headaches – to some degree bright lights really bothered me. I’d had a recent change in medication – I’m type 2 diabetic – so at first, I wondered if maybe it was because I’d made some medication changes.
Then uncharacteristically for me, I laid my head down on my desk at about 5:15 one Tuesday afternoon, and the next thing I know it was 6:15. I was super tired, and that just wasn’t me. By Wednesday I got tested and it was positive.
My wife also contracted it, despite the fact I took all precautions. My youngest son was living at home at the time and he also contracted it.
By day 10, [my wife and I] were relatively ill. We both ended up in the hospital for about five days in July, right in the middle of a major surge. We both received convalescent plasma, and my wife received Remdesivir.
I lost more than 20 pounds in this, and my wife was ticked off. I said, “Look, I don’t recommend it to anybody as a weight loss regimen!”
Despite the fact that we were [obsessive] about following all of the measures, even though we socially distanced and used masks and everything we were supposed to be doing, I still can’t nail down where I got the exposure. But it took me out of commission for a total of about four weeks. It took a while to get over the fatigue.
Any time that a physician becomes a patient is certainly an important experience because it gives us the patient’s view to those things that are going on around them, and it makes me a better physician to be a patient. All of us will probably be a patient at some point in our lives, and I think as physicians, it’s an important perspective and opportunity to reflect on how we put the patient at the center of all that we do, whether it comes to delivering care or crafting health policy.
Like in most crises, you try to see the silver lining. I think it’s made us all better physicians and better health care professionals – everyone on the allied health team – to have been through this, and to recognize things we can do better. We have certainly improved in our ability to care for this group of patients, and I see us in a position now to handle whatever comes down the pike.
Javier “Jake” Margo Jr., MD, family physician, Rio Grande City
About the 8th of August, a Saturday, I noticed post-nasal drip and assumed it was just allergies. It started triggering a cough but not too bad. By Tuesday, it was really bad, so I went to my allergist. [He] said, “This is COVID until proven otherwise.”
The family got tested at the hospital that day, and my daughter and I were positive – she had a little scratchy throat for, like, a day and then she was fine. My wife and son were negative.
Sunday morning, I went up to the hospital. I was just supposed to get plasma and go home, but there was a delay with the hospital receiving the plasma, so I got it around 5 o’clock. But because I had a fever, they wanted to keep me overnight to make sure it wasn’t a reaction to the plasma and to do some baseline labs in the morning if needed. I woke up Monday morning, my fever was raging, and I wasn’t magically better.
I started Remdesivir that day, and you couldn’t go home with it, so I was in the hospital for six days total.
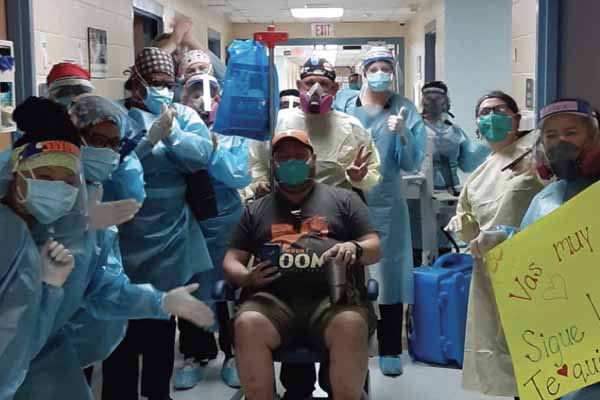
I went home that Friday, and like they had been doing for the other patients, they announced over the intercom that they had another successfully treated patient, and all the nurses and staff made a double file row almost like you’re coming out of the tunnel at football games. They rolled me out, and it was really neat: My staff and colleagues were all there waiting, and I didn’t expect to get emotional when it happened, but it really hit me. It meant so much.
Physicians are very self-critical, particularly when something doesn’t go the way we think it should’ve gone. And I kept asking myself questions like, “How did I get this? Where was I careless, even if I followed all the precautions?” At some point I came to the realization that it doesn’t matter. Odds are it was at work, and at some point when you’re in that type of situation you’re going to get it. And I think you have to be aware of that: There’s a risk involved, and we’re taking that risk every day. But this is our time to do what we’re trained to do.
So be kind to yourself. If we contract it, it’s not a failure on our part, and we shouldn’t look at it that way. Forgive yourself and try to smile a little more. We will get back to the days of handshakes and hugs. Know that it’s coming. Try to take delight in each day because each day really is a gift.
Tex Med. 2020;117(2):45-46
February 2021
Texas Medicine Contents Texas Medicine Main Page