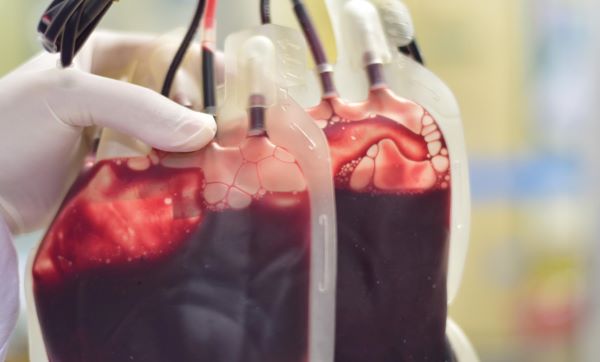
Trauma physicians in Texas almost couldn’t believe it when state legislators unveiled a landmark investment in prehospital whole blood during the 2025 session. The Texas EMS Alliance asked for $4 million and got $10 million instead. The medical community was issued a Texas-sized challenge, too – get whole blood onto every EMS unit in all 254 counties.
Now comes the hard part. Just what is exactly the best way to spend all that money, transform emergency procedures, and prove to the nation this statewide initiative can save more lives?
“It was amazing that we received the funding like we did,” said J. Lane Schnell, MD, a Tyler emergency medicine physician and chair of the Texas Medical Association’s Committee on EMS and Trauma. “There was a lot of support in that.”
There’s plenty of data to support having whole blood in the field. “Preferential whole blood transfusion during the early resuscitation period is associated with decreased mortality and transfusion requirements in traumatically injured patients,” summarized a 2024 study from the Whole Trauma Congress.
That’s certainly how Dallas-Fire Rescue sees it. The department launched a prehospital blood program in 2025, putting military-grade coolers with two units of whole blood on EMS supervisor vehicles in the city’s highest-trauma areas. Six months later, the number of supervisors carrying whole blood doubled. One year later, 34 out of 40 patients with life-threatening bleeding survived. Among them was a mother two months postpartum and multiple shooting and stabbing victims.
“Without the early intervention of the blood transfusion, the chances of survival are slim to none,” Dallas Fire-Rescue Chief Justin Ball told reporters in February. City officials are expanding the program to put whole blood within 10 to 15 minutes’ reach of patients anywhere in the city.
Now, there’s growing excitement across the state as members of the Governor’s EMS and Trauma Advisory Council (GETAC) determine how to disperse $10 million. Alan Tyroch, MD, an El Paso trauma surgeon, consultant to TMA’s Committee on EMS and Trauma and chair of GETAC, called it a “godsend” when the state allocated the funds.
All the work done to acquire this funding goes for naught if confidence bleeds out. Physicians should be watching how this program develops and support EMS and hospital teams, because this will take cooperation from all stakeholders, Dr. Schnell said.
EMS physicians and paramedics need to carry and use whole blood in the field. Hospital physicians need to use more whole blood in procedures. That triggers blood providers to stock more whole blood used predominantly by acute care facilities. The hospitals themselves must agree to the rotation and testing schedule to limit waste, multiple people interviewed by Texas Medicine said.
“There’ll be some growing pains as the program kicks off,” Dr. Schnell said. “But I think we’ll see this shift from giving the components of blood to giving whole blood, and I think that will simplify the matter.”
William Crews, MD, has a unique perspective as the medical director at Carter BloodCare in Dallas, the John Peter Smith Hospital blood bank in Fort Worth, and the Hendrick Regional Blood Center in Abilene. He’s also served on TMA’s Committee on Blood and Tissue Usage.
“A goal of the GETAC Prehospital Whole Blood Task Force is to get whole blood in every county. That sounds good until you realize, ‘Wait a second, we only have X number of blood donors that we can collect from,’” the Bedford pathologist said. “Can we meet the demand of this new effort to put whole blood on ambulances and still meet the demand of the traditional hospital, where blood has historically gone?”
‘Find a way to say yes’
Eric Epley, executive director of the Southwest Texas Regional Advisory Council and chair of the GETAC Prehospital Whole Blood Task Force, is a firm believer in low titer O+ whole blood. Were it up to him, every TMA member, EMS technician, and trauma physician in the state would start using it ASAP in emergency settings.
The American College of Surgeons estimates whole blood is used by 1% of EMS units in the country, including air medical units and ambulances. This $10 million funding haul is designed to expand whole blood usage and carriage all over Texas.
Finding whole blood in hospitals in Dallas, Houston or even Lubbock is relatively easy. It’s the “blood deserts,” as they’re known – the wide-open counties in rural areas – that can be tough.
On a Zoom call with program participants from around the state in February, Mr. Epley told members of task force and the chairs and executive directors of the 22 Regional Advisory Councils (RACs) that “there’s no second wave of funding.” This $10 million was given in a lump sum and has to stretch through August 2027.
“As far as I know, all the contracts [for the distribution of funds] have now been signed and fully executed,” Mr. Epley told Texas Medicine. His organization coordinates trauma systems across San Antonio and 22 South Texas counties and was the first regional deployment of prehospital whole blood. The San Antonio region now has more than 70 units on EMS or helicopters, the largest deployment in the nation. The money was held up by some bureaucratic hurdles, but “that’s all been resolved and now ready to be spent,” he said.
The Texas Department of State Health Services will work with the various RACs to distribute funding for blood acquisition, storage, and administration across EMS agencies that could not otherwise participate.
One key requirement is RACs will have to host blood drives, possibly numerous times based on area population. That got everyone’s wheels turning. At a March task force meeting, other ideas surfaced. What about asking hospital employees to give? Why not ask local school district employees? Perhaps two or three “walking blood banks” can be stood up, a call-to-action taken straight from the military.
“I’m really interested if we’re going to try this, that we find people who find a way to say yes,” Mr. Epley told members at the March meeting.
Mr. Epley, a paramedic with three decades of flight and tactical experience, is passionate. But some of the initial problems involve troubleshooting logistics. Mr. Epley said the first major purchases will be equipment – specialized coolers that can keep blood between 1 to 6 degrees Celsius, a strict narrow range to maintain cell viability and prevent bacterial growth. Some coolers have built-in monitors and alert systems, so providers can learn in real time if blood is becoming warm.
In rural Texas, there’s not a Level I trauma center anywhere close to typical one stop-light towns. Out in the hinterlands, patient transport times could be anywhere from 45 to 90 minutes, Dr. Schnell said. His hospital, UT Health Athens, offers Level IV trauma support, emergency care, and a thriving labor and delivery practice. It’s the only such hospital in Henderson County.
So how much whole blood should any EMS agency disperse at any given time? It’s a delicate balancing act. Blood centers typically take their supply-and-demand cues from the hospitals, Mr. Epley says.
“We should only issue whole blood to the field that can be used at the tertiary centers each week,” Mr. Epley said. “The limiting factor for prehospital whole blood relies completely on physicians and hospitals to use emergency release whole blood to increase the ‘demand’ signal to the blood centers. Otherwise, wastage will skyrocket.” The San Antonio model currently has more than 70 units in the field but less than 2% wastage, Mr. Epley says.
B.J. Smith, the chief operating officer of Carter BloodCare, said the blood centers in Texas are in “complete agreement” with GETAC’s mission. As nonprofit entities that rely solely on volunteer donations, blood centers have “a heartfelt and strong sense of stewardship to make sure that all the blood that is given to us is utilized,” he said.
Carter BloodCare is the largest blood center in 59 Texas counties. It’s a balancing act to make sure this push for prehospital whole blood doesn’t cannibalize what’s needed in the acute care settings, Mr. Smith says.
“If we were to respond to every agency that wanted it, we do not have hospitals willing to take it,” Mr. Smith told Texas Medicine. “It’s a growth curve. It’s going to take education, cooperation from the acute care setting all the way back to the EMS setting.”
Taking the initiative
Out in rural Texas, blood providers and EMS directors must monitor the hospital’s inventory levels based on usage, Dr. Schnell said. For most EMS agencies and blood centers, switching to whole blood usage is a new procedure that requires an all-in commitment.
“There’s a lot of regulation and caution around storing, releasing, and administering those blood products,” Dr. Schnell said. “And from a regulation standpoint, it’s a whole new process. It’ll create some strain and some difficulty for the blood banks. I think ultimately our patients will be better served.”
Carlos Palacio, MD, a member of the TMA Committee on EMS and Trauma and the whole blood task force, said his hospital in McAllen started new whole blood procedures in 2019. Using whole blood at the time wasn’t fully accessible. Other hospitals needed to be convinced it was a beneficial product, he says. As of March 2026, 53 counties in Texas have whole blood initiatives, according to the Prehospital Blood Transfusion Coalition.
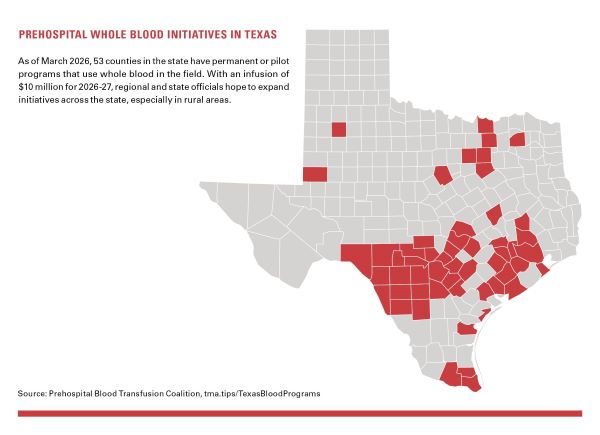
“I can tell you at the beginning, people didn’t want to participate,” the McAllen critical care surgeon told Texas Medicine. “Some of it was contractual obligations they had. It was a challenge.”
As more agencies started seeing the benefits, more whole blood was put into circulation in South Texas, says Nathan Ramon, executive director of Trauma Regional Advisory Council-V in Harlingen.
“Rather than just getting more whole blood available, I think it’s also making sure you have people that are committed to the cause, getting them on board,” Mr. Ramon told Texas Medicine.
In the Alamo City, experts are shouting from the hospital rooftops about the importance of whole blood usage in the field.
In San Antonio’s program, which launched in October 2018, EMS providers store whole blood for up to 14 days. Any unused units were sent back to South Texas Blood and Tissue, then to University Hospital’s trauma bay for use over the next 15 to 35 days. As a Level I trauma center, University Hospital has no problem taking unused blood from EMS units and using it on patients. On average, the trauma unit has over 8,000 trauma admissions patients per year and has administered over 15,000 units of low titer O+ whole blood.
Mr. Epley said TMA member physicians can have a major impact on the program’s success by doing one thing. “What we really need from trauma surgeons, general surgeons, obstetricians, and emergency medicine doctors that care for all bleeds that need emergency release transfusion is to start using low titer O+ whole blood,” Mr. Epley said. “When you do, the patient will do better, and you indirectly support the prehospital whole blood effort across the state.”
Donald Jenkins, MD, a trauma surgeon with UT Health San Antonio and University Hospital, calls this the “great limiting step in the whole process.”
“If we don’t have hospitals that will use the blood that EMS had in their possession but was unable to use, there is high potential for high wastage,” Dr. Jenkins told Texas Medicine. “As those blood producers start to gauge the use rate and the tempo, then they can get a better handle on our par level to make sure we have high utilization and avoid high waste.”
More data will be collected as the $10 million gets spent and more whole blood is dispersed statewide. This isn’t an issue that’ll be solved in a few weeks or a few months. Legislators will want reports about their funding, and they’ll want to hear physician and patient success stories.
“The No. 1 barometer for success would be can we prove that lives were saved by putting whole blood on ambulances or making the effort to get whole blood on ambulances across the state,” Dr. Crews said.
So, what constitutes success?
“As a clinician and physician, I would say if you save one life, it’s worth it,” Dr. Schnell said. “But especially based on what San Antonio has seen, there have been multiple lives saved. I think as we ramp this up and roll it out throughout the state, we should see a significant decrease in mortality, and that’s something that’s measurable.”