Two recent studies suggest expanding Medicaid will not only save Texas money, but add to the Lone Star State’s coffers.
With another opportunity for the Texas Legislature to debate Medicaid expansion on the horizon, the Texas Medical Association sees the Episcopal Health Foundation reports as evidence to support efforts to expand meaningful coverage for the state’s poor and vulnerable populations.
One report found that a “fully operational, 90% federally financed” Medicaid program – as originally envisioned under the Affordable Care Act (ACA) – would save the state more than $50 million per year, or nearly $110 million over a biennial budget.
“Conceptually, the idea that the state spends money in an inefficient way, and could spend money more effectively to get better coverage for more Texans in a way that is more cost-effective for the taxpayer in the state of Texas, it’s a no-brainer,” said Austin pediatric cardiologist Hanoch Patt, MD, a member of TMA’s Select Committee on Medicaid, CHIP, and the Uninsured.
“The term Medicaid expansion has been a very hot-button political issue in the state, but ultimately, having coverage and access to care for vulnerable Texans shouldn’t really be a political issue. It should be an issue of what’s the right thing to do in the state, and how do we do that most effectively at the lowest overall cost and the most cost-effectiveness for the taxpayer in the state of Texas.”
A second study focusing on the county-level impact of Medicaid expansion estimates the move would result in more than 950,000 newly eligible adults enrolling in Medicaid, $5.4 billion in annual federal dollars, and “favorable” implications for both state and local governments.
Twelve remain
The Episcopal Health studies, released in September, aren’t the first to project a positive fiscal impact if Texas expands Medicaid. Helen Kent Davis, TMA’s associate vice president of governmental affairs, says the new reports are in line with past examinations.
“The report used similar modeling that others have used and a conservative estimate in terms of the percentage of eligible population that will be enrolled and per-enrollee costs,” Ms. Davis said of the Episcopal report focusing on the impact of 90% federal assistance. “It’s a solid estimate; of course, any kind of prediction of the future is difficult. But a growing body of research shows that improving health care coverage not only improves the financial health of enrollees but also state and local governments.”
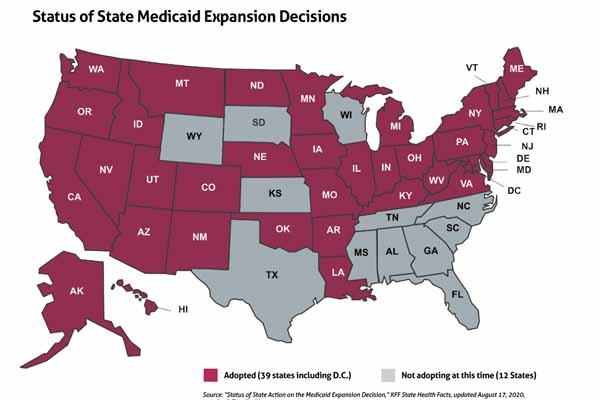
Texas is one of 12 states that have not expanded Medicaid, according to the Kaiser Family Foundation. (See map, page 24.)
TMA policy supports state leaders and lawmakers coming up with a Texas solution for expansion that
“[d]raws down all available federal dollars to expand access to health care for poor Texans.”
At a virtual meeting of the TMA House of Delegates on Sept. 12, delegates referred a resolution on Medicaid expansion to the Board of Trustees for action. That resolution called on TMA to advocate for a statewide ballot measure on Medicaid expansion, and to encourage a dialogue on Medicaid expansion as a vehicle to reduce the state’s high uninsured rate.
Earlier this year, Oklahoma and Missouri approved state ballot initiatives for Medicaid expansion.
If two-thirds of lawmakers in both the Texas House and Senate approve a joint resolution to advance a constitutional amendment, Texas voters would have the chance to decide. Or, the legislature and governor could pass legislation on their own to expand Medicaid.
Cost and savings
One of the Episcopal Health studies (tma.tips/ehfmedicaid1), conducted by a trio of researchers including members of the Austin government affairs firm Texas Star Alliance, specifically looks at the impact of one aspect of Medicaid expansion: The transfer of significantly more funding responsibility for the program to the federal government.
The report “assumes a ‘normal’ coverage environment rather than one marked by unusual activity, such as the unemployment spikes and health care delivery disruptions caused by the coronavirus pandemic, because it would take several years to implement a coverage expansion and, by then, the pandemic and its attendant recession are likely to be over.”
In such “normal” times, without expansion, the federal government covers 62% of Texas’ Medicaid funding, with the rest coming from state and local revenue, the report states. If the state grew its Medicaid pool to include adults ages 19-64 with incomes below 138% of the federal poverty level, federal funds would take care of 90% of the program’s funding.
Researchers add that traditional Medicaid expansion – offering benefits under the current program to more low-income people as specified under the ACA – isn’t the only way for the state to extend coverage to that group.
“As shown by the experience of other states, such as Indiana, the state has flexibility in how to take advantage of that opportunity, including the creation of a plan that aligns with state priorities such as personal responsibility, budget certainty, and benefits more in line with the commercial market,” the Episcopal report said.
Using a 2013 fiscal note from the Texas Legislature that looked at the impact of Medicaid expansion, and updating those numbers for population growth, the study estimates 1 million Texans would enroll in expanded Medicaid at a cost of $525 per enrollee per month, or $6.3 billion total per year, of which the state would chip in $650 million.
There are two ways the state could pull that money together: through cost savings to existing health programs and increased tax revenue collected from health plans.
If some patients in existing state programs were to receive coverage through a federally funded Medicaid expansion instead, the study projects the state could save:
•$106 million on existing services for pregnant women and women needing treatment for breast or cervical cancer, which currently are funded through the Healthy Texas Women program; and
•$488 million within health programs funded with general revenue, which include community mental health services; inpatient care of incarcerated prisoners; substance abuse treatment services; HIV medication assistance; and the Kidney Health Care program.
That $594 million in combined savings – plus additional revenue from existing taxes on state-licensed health plans and HMOs totaling $110 million – would net $704 million in annual savings, researchers calculated.
“Compared to the $650 million cost of expanding coverage, this is a positive difference of $54 million per year or almost $110 million for the biennial budget,” the report said. “If the state were to find a new funding source, then $704 million annually or just over $1.4 billion for the biennial budget could be redirected to other budgetary priorities. A number of states have done that with financing mechanisms that include premium or insurance taxes, provider assessments, lottery proceeds, and increased sales, cigarette, and alcohol taxes.”
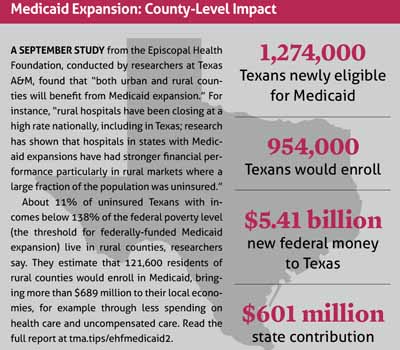
A separate, county-level report looks at estimates for all 254 Texas counties of how many adults would likely be eligible for expanded Medicaid, and how many actually would enroll. (See “Medicaid Expansion: County-Level Impact,” page 26.)
“Look at the data”
With the next Texas legislative session just months away, Dr. Patt notes that expanding access to care in Medicaid is a two-pronged approach: Along with increasing coverage, there’s also “figuring out a way to pay providers, especially ambulatory outpatient providers” while discouraging more expensive care.
Lawmakers denied TMA’s aggressive push during the 2019 legislative session to increase long-stagnant Medicaid physician payment rates.
“Policymakers should be open to different approaches, and look at the data, and look at what opportunities there are to redirect funds in a way that will save money,” Dr. Patt said. “We all understand that hospital and emergency room care is very expensive, and if the state does a better job through payment rates, through other mechanisms of encouraging outpatient care, care at the right time, right place, that it will ultimately save the state money.”
Tex Med. 2020;116(11):25-29
November 2020 Texas Medicine Contents
Texas Medicine Main Page