
The mental health fallout caused by COVID-19 radiates throughout Texas, with the most severe damage occurring where the virus hits most directly.
“Entire families are affected,” says James Castillo, MD, an internist who provides palliative and hospice care in the Rio Grande Valley. “I’ve had so many families with both parents dying at the same time. And having conversations with those people about end-of-life wishes and goals when they just lost one parent last week, and now they’re facing a repeat of the exact same scenario, that’s really, really difficult to tolerate.”
In a pandemic marked by the steepest economic downturn since the Great Depression, people don’t need COVID-19 preying on their state of mind as well as their body, says Alex Kudisch, MD, a psychiatrist and medical director for the geriatric behavioral unit at Valley Baptist Hospital in Harlingen.
“Loss of job, loss of insurance, loss of housing, loss of access to health care – all of that plays into the patient’s mental health,” said Dr. Kudisch, also medical director for BRC Recovery in Austin, which provides substance abuse counseling.
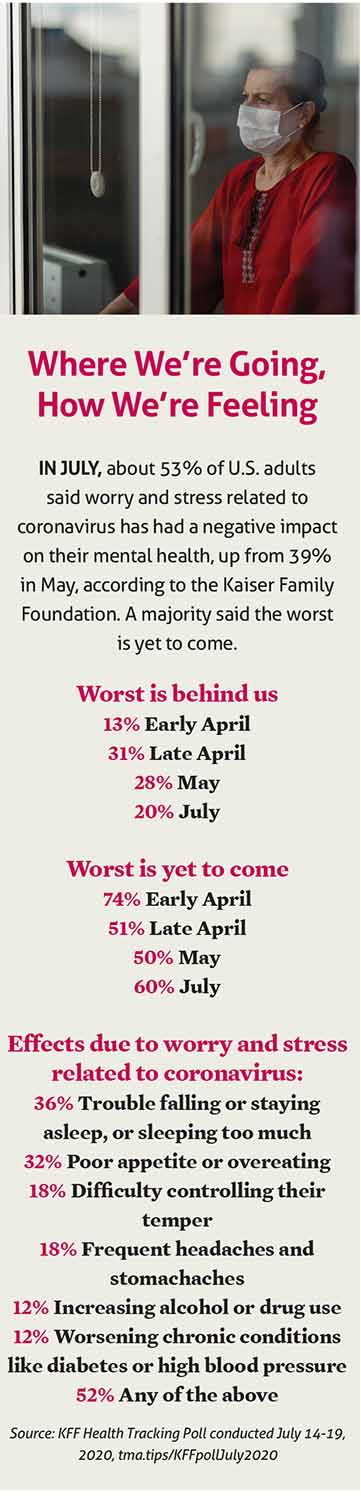
In fact, growing numbers of people are saying that worry and stress related to coronavirus have negatively impacted their mental health, according to a Kaiser Family Foundation (KFF) poll. (See “Where We’re Going, How We’re Feeling,” page 24.)
“Anxiety, depression, and substance use are the major three diagnoses we see of those that are primarily anxious about COVID or have had COVID and are dealing with the mental health comorbidities,” Dr. Kudisch said. But, he added: “Everything is magnified as if it were on steroids in a sense – all the psychiatric diagnoses.”
Thanks in part to advocacy by the Texas Medical Association, the Texas Legislature increased mental health spending in the last two sessions (www.texmed.org/CPAN). However, the state still has had to face the pandemic with critical unmet mental health needs.
In September 2019, 12.5 million of the state’s roughly 29 million people lived in federally designated mental health professional shortage areas, according to KFF.
“We’re chronically underserved when it comes to mental health,” Dr. Castillo said.
It will take months to years for scientific studies to demonstrate the full impact of the pandemic on Texans’ mental health, according to an April 28 report by the Texas-based Meadows Mental Health Policy Institute.
“Most mental health impacts of trauma manifest 60 to 90 days following exposure to traumatic events, though the sustained and unpredictable length of the COVID-19 pandemic stressors may change that pattern,” said a summary of the report (tma.tips/MeadowsReport2020). “These effects can continue to significantly manifest for years, as seen following Hurricane Harvey.”
But there have been encouraging responses to the crisis, starting with the rise in telemedicine, says Thomas Kim, MD, an Austin psychiatrist and internist who has run several telemedicine programs.
For decades, telemedicine had been stymied by artificial barriers such as the lack of payment parity between an in-person office visit and a telemedicine visit, he says.
“Those barriers have been taken down to a large degree, and more and more of my peers are embracing these technologic tools to create a robust and meaningful encounter [with the patient],” Dr. Kim said.
Here are four of the biggest mental health challenges physicians see Texas facing because of the COVID-19 pandemic.
 “Terrible and scary” mental symptoms
“Terrible and scary” mental symptoms
COVID-19’s physical symptoms, like a dry cough, are well known. But the disease itself also causes anxiety, depression, dissociation, disorientation, panic attacks, psychosis, and hallucinations, Dr. Kudisch says. That is typical of diseases that generate high fever and attack major organs, he says.
“We don’t really have a COVID psychiatric syndrome or neurological syndrome,” he said. “It’s just what we understand to be symptomatic of [abnormal health]. If your kidney’s malfunctioning, your brain is also.”
That malfunctioning can traumatize patients, Dr. Castillo says.
In March, he had an older patient who beat the odds and came off a ventilator alive. Despite this success, the previously healthy man was delirious and encephalopathic during the first week, Dr. Castillo says.
“He remembered [the delirium] as really terrible and scary,” he said.
Though never hospitalized, Waco family physician Tim Martindale, MD, got a taste of what COVID-19 can do to a person’s mental state when he contracted a severe case in April.
“About day six or seven, I got hit with terrible panic attacks that I’ve never actually experienced before – just the sense of your heart racing and your lips numb and your mind racing. … and it went on all through the night,” he said.
Even patients with mild cases of COVID-19 may need regular counseling and reassurance to help them through these symptoms, Dr. Martindale says. He had to call up relatives and fellow physicians to talk him through the powerful anxiety that hit him about eight to 10 days into the illness.
This emotional experience prompted him to counsel others in the months since he has recovered. He speaks by telephone daily to up to 15 people who are sick with COVID-19 – some his patients, others not – about the physical and psychological symptoms they face.
“Sometimes, COVID-19 patients need a listening, relatable ear more than anything else as they cope with the disease,” he said.
Substance use and suicide
Drug and alcohol misuse have taken off since the pandemic hit the U.S. in March. There was an 11.4% year-over-year increase in drug overdose deaths in the first four months of 2020, according to an analysis by the U.S. Office of National Drug Control Policy. Meanwhile, U.S. alcohol sales surged 27% between March and June, says CNN.
“[People are] using drugs and alcohol to self-medicate the symptoms that they’re having for anxiety,” Dr. Kudisch said. “Why? Because they can’t go to the movies when they’re stressed. Or they can’t go to the mall and walk. So they’re stuck pretty much at home. And alcohol is easy and very accessible.”
This increased use pushes some toward addiction and makes it harder for others who struggle with drug or alcohol use disorder to stay sober. COVID-19 can disrupt substance use treatment and group therapy (such as Alcoholics Anonymous), cause greater isolation, and make people afraid to seek treatment at a hospital for fear of infection, according to the U.S. Centers for Disease Control and Prevention (CDC).
“Maybe they were diagnosed with depression in the past and that’s heightened, or they’ve been experimenting with alcohol and now they’ve got full-blown binge substance use,” Dr. Kudisch said. “They were experimenting and now they’re using larger amounts.” (See “Opioids: The Forgotten Epidemic?” page 32.)
The anxiety and isolation caused by COVID-19 also seem to be causing an increase in suicides, Dr. Kudisch says, based on personal observation, not published studies.
“In the emergency rooms we certainly do see more frequently the suicide attempts, overdosing, or suicidal thinking,” he said “They’re not necessarily carrying out a plan yet, but [having a history of depression], they’re now suicidal and they come in for treatment or help, or their family members bring them in.”
In late June, 40% of U.S. adults said they struggled with mental health or substance use issues, with 11% of those people seriously considering suicide, according to a CDC survey. The survey showed even higher risk for suicide among certain groups, including 18- to 24-year-olds (25.5%), Hispanics (18.6%), Blacks (15.1%), self-reported unpaid caregivers for adults (30.7%), and essential workers (21.7%) (tma.tips/CDCCovidJuneSurvey).
In 2018, 3,930 Texans died by suicide and 3,005 died by accidental drug overdoses, according to CDC. Unless the state improves its efforts to detect and treat depression and addiction, every 5 percentage point year-over-year increase in the unemployment rate could lead to 300 more deaths by suicide and 425 more deaths from drug overdoses, according to the Meadows Mental Health Policy Institute.
With TMA support, the Texas Legislature made strides toward addressing mental health and suicide in the 2019 session, particularly among young people, who have the fastest-growing suicide rates of any age group in the state. Lawmakers also directed state agencies to analyze state and regional suicide trends and review Texas’ suicide prevention initiatives (tma.tips/Texas2020SuicideReport).
Getting around isolation
The most effective tool we have against COVID-19 – isolation – comes with its own serious side effects.
Many patients of Dallas psychiatrist Leslie Secrest, MD, live in nursing homes, where since March patients have been separated from each other and often denied visitors.
“Those folks at times describe it as almost as if you’re incarcerated,” he said. “You can’t have visitors, you are quarantined. … You get in this effort to keep people safe, but [they] don’t have the emotional support of having a conversation day in and day out. And that whole population has sort of been forgotten about.”
Hospitals face an even more serious situation, Dr. Castillo says They typically put COVID-19 patients in isolation wards to prevent the spread of the disease. While necessary, these wards can become a breeding ground for depression among patients, he says.
“You’re hearing ‘Code Blue, Code Blue,’ seeing patients getting intubated, all the hustle and bustle, doctors talking, maybe other patients being confused,” he said. “[Hospitals are] not the most peaceful of places, and when it’s a disaster like this type of situation, that’s only magnified.”
Telemedicine is usually the only practical way to safely open up a patient’s world to family and friends, Dr. Castillo says.
“Even when someone is on life support, most families still want to say goodbye, even if the person can’t respond to them,” he said. “They can hear their voice and they can see them. … That’s helped some families have some sort of closure.”
However, telemedicine has limits, especially when it comes to discussions about end-of-life plans or directives, says Robert Fine, MD, a member of TMA’s COVID-19 Task Force and clinical director of the Office of Clinical Ethics and Palliative Care at Baylor Scott and White in Dallas.
“One of the things we’ve found on the acute care side of things is that it’s very hard to have end-of-life conferences via Zoom,” he said. “Families were often paralyzed at making decisions. And once we got the family to the bedside with all the PPE (personal protective equipment), the decisions were made [by family members]. That’s when we realized that ...we’ve been too strict. We need to let people in for these end-of-life conversations.”
In August, TMA and six other Texas health care organizations produced a set of principles designed to guide hospitals and other health care facilities toward greater flexibility in visitation policies for patients facing serious illness or end-of-life situations during the pandemic. (See “Flexibility Needed for End-of-Life Visits,” right.)
That flexibility can help give families and the patient peace of mind, Dr. Castillo says. In-person visits to dying patients have to be weighed carefully because they require extra PPE and valuable staff time, but he tries to do them whenever possible.
“We had one patient who was in his 30s with Down syndrome, and he developed severe [COVID-19] and he was dying,” Dr. Castillo said. “And that’s the mom’s baby, you know. She wanted to be with him, she wanted to hold his hand.”
For patients who are ill but not clearly dying, physicians might consider some non-human companionship, says Chelsea Clinton, MD, a rheumatologist in San Antonio. Early in the pandemic, some research indicated that pets like cats and dogs might spread COVID-19. CDC now says the chance of spread from animals appears to be low, though more study is needed. For quarantined patients struggling with high anxiety levels, the benefits of seeking the company of a pet may outweigh the risk, Dr. Clinton says.

Treating patients with mental illness
Texas traditionally lags behind most other states on mental health care. It currently ranks 38th among the 50 states based on the prevalence of mental illness and access to care, according to Mental Health America (tma.tips/TexasMentalHealthRank).
But the COVID-19 pandemic has opened up a range of new and complicated problems for treating Texans with existing mental illness. For instance, they struggle more than ever to get into psychiatric hospitals when they need in-patient treatment, says Dr. Secrest.
COVID-19 is not the only reason, but it has played a big role, he says. For example, the number of rooms available has been reduced because patients can no longer share them.
Also, psychiatric hospitals often are not set up to take patients with serious physical illnesses, Dr. Kudisch says. For instance, patients cannot have IVs in many cases because they pose strangulation risks.
All this forces emergency departments at local general hospitals to hold patients longer when they’re in distress, Dr. Secrest says.
“One of your nightmares is to be in an [emergency department] and have a patient who is psychotic and agitated,” he said. “That can be really quite disruptive.”
Delaying or denying in-patient psychiatric hospitalization also makes treatment more difficult and drawn out, Dr. Kudisch says.
“So I’m having to see them and stabilize them [at a general hospital] when you would normally treat them in a psychiatric hospital,” he said. “They should be in the setting where they’re getting the psychological therapies, the attention of those facilities. So I think that’s something we need to work on still.”
Patients with mental illness also have greater difficulty finding places to go once they leave the psychiatric hospital, Dr. Kudisch says. Nursing homes and homeless shelters are no longer an option for mentally ill people because they are turning people away to prevent spreading COVID-19.
In some cases, recovered COVID-19 patients are stigmatized by their community or family because they’ve had the disease.
“The optimal thing, of course, is for [the patient] to go home,” Dr. Kudisch said. “But then many times the family members are afraid they’ll get sick, and they’re afraid the patient has been exposed maybe to COVID [in the hospital]. So the families are not wanting to take them back.”
Fortunately, telemedicine has emerged at the same time as a way for physicians to help COVID patients cope with these and similar problems. It allows physicians to respond more nimbly to urgent situations and provide supportive treatment in almost any setting, Dr. Kim says.
“The true value of telemedicine, and health care in general, is having the right doctor with the right information at the right time,” he said. “If we manage to satisfy all three, I think we will see enormous value for the effort to sustain a state of wellness long after this pandemic has subsided.”
COVID-19 Mental Health Resources
Texas Medical Association Tips and Strategies for Helping Patients Manage Distress: tma.tips/COVIDbehavioralhealth
Texas Department of Health and Human Services 24/7 COVID-19 Mental Health Support Line: (833) 986-1919
TMA podcast with Austin psychiatrist Thomas Kim, MD, designed to help physicians deal with the stress of COVID-19.
Tex Med. 2020;116(10):18-25
October 2020 Texas Medicine Contents
Texas Medicine Main Page