The “whoop” that gives whooping cough its name is a terrifying sound. It’s the sound of someone — usually a child — gasping for breath.
In 1914, a vaccine for the bacteria that causes pertussis finally offered protection. In the 1940s, the vaccine was combined with those for tetanus and diphtheria to create what eventually became the DTaP (diphtheria, tetanus, and acellular pertussis) vaccine widely used today. A booster — the Tdap — follows around age 11 or 12. Adults, especially pregnant women and people who will be around babies, should receive an additional Tdap booster.
Since widespread use of the pertussis vaccine began in the 1940s, incidence of the disease has dropped more than 80 percent, the U.S. Centers for Disease Control and Prevention (CDC) reports.
But pertussis has made a resurgence. Between 1975 and 1985, nationwide cases hovered between 1,000 and 3,600 a year. In 2003, cases broke the 10,000 mark, peaking at 48,277 in 2012, and dropping to 17,972 in 2016, according to CDC.
Anti-vaccine sentiment is certainly part of the problem. Also, a 2018 study in Science Translational Medicine showed a new pertussis vaccine introduced in the 1990s has fewer side-effects, but wears off more quickly, even with the booster.
Those factors allow pertussis to spread, especially in school children. But vaccination still remains the best protection.
Download a printable copy of the infographic below.
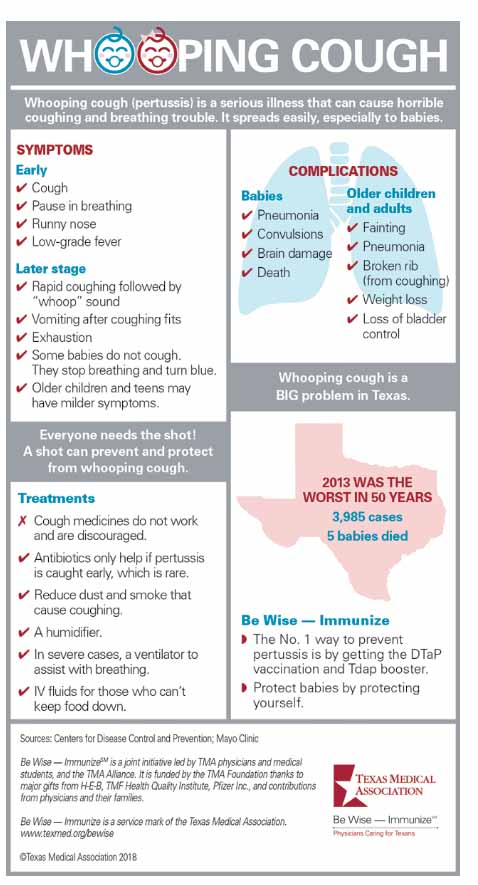
Tex Med. 2018;114(11):47
November 2018 Texas Medicine Contents
Texas Medicine Main Page