Physicians get asked about COVID-19 all the time, and many questions are tough to answer, particularly because so many things about the disease are still unknown.
But after looking at some recent trends, Texas Medicine Today staff had a few questions of our own.
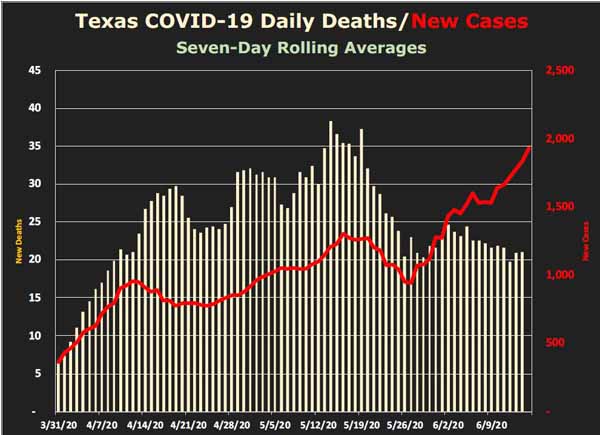
For example, since late May, the number of daily new COVID-19 cases in Texas (based on a seven-day, rolling average) has risen substantially – from a little over 1,000 to more than 2,200 on June 16. The number of daily hospitalizations also has spiked in recent weeks. However, the number of daily deaths has declined during that time.
What’s driving these numbers?
Texas Medicine Today reached out to several leading public health experts to try to make sense of the data and find out what the numbers are telling us about that current status of the pandemic in Texas.
Why are COVID-19 cases, hospitalizations, and test positivity rising while deaths are declining?
A definitive answer remains unclear, “but any time we’re seeing one particular number go up we’re concerned because there will be a correlation [with the other numbers] at some point,” said John Carlo, MD, former medical director for Dallas County Health and Human Services and immediate past chair of the Texas Public Health Coalition.
That correlation could become clear in a week or two, says Robert Haley, MD, a Dallas epidemiologist. That is because case numbers, hospitalizations, and test positivity are leading indicators while deaths are a lagging indicator of the disease’s spread, he says.
In recent weeks, social distancing and mask-wearing have declined as businesses have reopened, and more Texans have begun venturing out of their homes, including during the Memorial Day holiday.
In addition, on Tuesday, Gov. Greg Abbott cited several factors such as an increased number of people under 30 testing positive and one-time spikes in certain counties where prison inmates’ positive tests all came back at once.
Factors like those “may not seem like much” by themselves, but they’re all aggregate contributors, John Zerwas, MD, executive vice chancellor for health affairs of the University of Texas System and one of four physicians on the state’s COVID-19 strike force, told Texas Medicine Today.
“Memorial Day was the beginning of a lot of that, where we saw a lot more social interaction, if you will,” Dr. Zerwas said. “The observation has really been that we’re not seeing the level of mitigating behaviors that we need to see to really combat the epidemic. That’s social distancing … masking, and just good hand hygiene.”
However, there may be another explanation for the lag between the number of deaths and the other data, says James T. McDeavitt, MD, senior vice president and dean of clinical affairs at Baylor College of Medicine. He also runs Baylor’s incident command center for emergency response.
It’s possible that older Texans – those most likely to die once infected with the coronavirus – have gotten better at protecting themselves from the disease through social distancing and mask-wearing, Dr. McDeavitt says. That might also help lower the number of deaths.
Are younger, healthier people getting sick now?
This also could explain why deaths are declining, because younger people are less likely to die from COVID-19 – even, according to a June 15 report in Morbidity and Mortality Weekly Report, among those who are hospitalized and admitted to intensive care.
Earlier this week, Governor Abbott scolded people in their 20s for not wearing masks. He based this on anecdotal information from local health departments and county judges around the state, though no confirmed data were available at the time, according to the Dallas Morning News.
However, the spread of COVID-19 among young people might not be attributable only to casual mask use or poor social distancing, Dr. Carlo says. People in their 20s also are heavily represented among the “essential” workers who hold jobs that frequently deal with the public, he says.
“We’ve definitely seen higher numbers of people hospitalized in the Dallas area among those who have occupations that have been called essential,” Dr. Carlo said.
Is the virus changing to become less lethal?
“This virus is not becoming less lethal,” said Umair Shah, MD, executive director of Harris County Public Health. “This virus is just as lethal as it has been before. The concern is for every age range, whether you are a child, or you are a senior, whether you’ve got underlying health conditions or not. In the meantime, all of us continue to be at risk. It’s really about exposure.”
Is treatment changing? Are Texans getting treated sooner?
Remdesivir is the only drug cleared by the Food and Drug Administration to treat COVID-19, and it shows some promise in helping patients, says Dr. McDeavitt. However, the biggest advances in patient treatment have been improved intensive care procedures, Dr. Haley says.
For instance, hospitals now treat many patients on their stomachs instead of their backs to help them breathe better, he says. Physicians also have a better understanding of the optimal time to put a patient on a ventilator.
“Early in the epidemic, [intensive care units] all over the country were reporting a 50% to 75% mortality rate for anyone who went on a ventilator with this disease,” Dr. Haley said. “At the Parkland ICU, they’ve got it down to 25%, which is remarkable. And they ascribe that to increased practice and tremendous proficiency of our ICU nursing teams.”
Also, Texas hospitals are not overwhelmed with patients – as hospitals were in places like Italy and New York – and that means the treatment here is more likely to save lives, Dr. Carlo says.
Why do all the models predict such different results?
Models showing a disease’s spread rely on the information programmed into them, Dr. Haley says. If the information makes accurate assumptions, the model may be more accurate. If the assumptions are not accurate, it won’t be.
However, models are not a way to predict the future, he says. They’re a guide to show what might happen in different scenarios, such as what the disease’s spread will be like if most people wear masks compared with most people not wearing masks?
Also, scientists have never before tried to model the behavior of a pandemic in real time, Dr. Carlo says. It’s difficult to construct an accurate model when so much about COVID-19 – and people’s reactions to it – remains unknown.
“We’re somewhere in the middle [of this pandemic],” he said. “It’s very hard to apply a model in a system where we don’t even know where we are.”
Are the big cities preparing – or overreacting?
Many mayors and county judges in Texas’ largest metropolitan areas have publicized coronavirus “alert levels” and pushed Governor Abbott to impose strict virus-protection measures, such as requiring people to wear masks in public. Leaders in less-populous areas, which have far fewer COVID-19 cases, have been less likely to advocate such approaches.
It’s hard to generalize about the preparedness of Texas cities, Dr. Carlo says. Some have tried hard to combat the virus aggressively while others have taken a more hands-off approach.
However, hospitals in big cities have mostly created emergency plans to meet the challenges of COVID-19, Dr. Haley says. For instance, hospitals in Dallas have contingency plans to expand their ICUs on an emergency basis, and they’ve created emergency backup teams, he says.
Likewise, Baylor in Houston made extensive preparations for sharp spikes in the rates of COVID-19 early in the pandemic, Dr. McDeavitt says.
“We were seeing hospital systems fail [in other cities and countries],” he said. “I don’t think it was an overreaction to prepare for potential catastrophic health system failure. And we did. We developed surge plans and surge capacity and staffing plans, training systems for physicians to up training and take on new roles.”
Dr. Shah also points out: “I think what we have to remember is that ultimately, especially in urban communities, we have to do everything we can to fight this pandemic. What you’re seeing now is local officials again trying to make the case that there’s an importance on how things are playing out in larger communities, urban communities, differently than the rest of the state.”
Could the difference between data on deaths and data on illnesses be caused by political manipulation or errors?
Political manipulation of the data seems unlikely, the physicians agreed. But mistakes in the data are possible Dr. Carlos says.
“I think there’s always the risk that there could be errors in the data capture,” he said. “It would not be surprising to have [discrepancies] in terms of the data collection simply because things are happening so quickly, as well as the massive amount of information that’s going into this.”