
The hubbub was loud and happy – but nervous – in the seconds before fourth-year medical students at The University of Texas Rio Grande Valley (UTRGV) School of Medicine opened their Match Day envelopes.
Forty-five students in the school’s fourth graduating class, along with their family members, friends, and UTRGV officials, gathered at the school’s performing arts center in Edinburg to discover where they would train as resident physicians.
The UTRGV Match Day event was mirrored at 12 other schools in Texas with graduating classes and 191 across the country. Every third Friday in March, the National Resident Matching Program (NRMP) sends medical students who have matched an envelope to be opened right at 11 am CT.
As luck would have it, this Match – held coincidentally on St. Patrick’s Day – was again the biggest in history for total number of positions offered. This was the 22nd consecutive year the Match could claim the largest number of total positions in the program’s history, according to NRMP.
This match was also special in that this class of medical students spent their entire four years in the shadow of COVID-19. UTRGV, like other medical schools, found ways to offer classes online and reintegrate students back into clinical work. But it took time and made the famously stressful medical school experience that much more stressful.
“I learned in the military a long time ago ... a saying that I keep with me: adapt, improvise, and overcome,” UTRGV School of Medicine Dean Michael B. Hocker, MD, told the students as they were waiting to open the envelopes. “I couldn't say we have a more resilient group of medical students who have really improvised, adapted, and overcome over the last four years.”
Once a faculty member announced the 11 o’clock hour, some students ripped open their envelopes as soon possible. As they did, the auditorium filled with shrieks of joy, hugging, and high-fives.
Other students, like Jose Benitez, hesitated a minute or two before discovering the next step in their journey as a physician.
“I was a little nervous,” he explained later. “You really don’t know what you’re going to get. Anything is a blessing at that point, but there are some [residency] programs that are further away from family. All programs have different qualities and strengths, so there’s a lot of thought process in selecting your top programs. It definitely is a little nerve-wracking.”
Mr. Benitez stood before a rapt audience of his mother, brother, sister, and nephew, all wearing T-shirts announcing their support for him. When he did open the envelope, the news was good. He got one of his top choices – an internal medicine residency at UT Health San Antonio.
“It was the first interview, and I was pretty convinced that I wanted it in my top three even then,” he said. “I’m definitely very happy with the results.”
Aside from training him as a first-generation physician, the residency will accomplish two personal goals. It will keep him close to family and make it easier for him to return to the Rio Grande Valley – where he grew up in Mission – to practice as a physician.
Those plans are music to the ears of faculty members like Leonel Vela, MD, senior associate dean for educational resources. UTRGV School of Medicine is one of the state’s newest medical schools – opened to students in 2016 – and was created in part to help bring physicians to one of the state’s poorest and most medically underserved regions.
“This medical school was established with a dream that the whole Valley had that goes back generations,” he said.
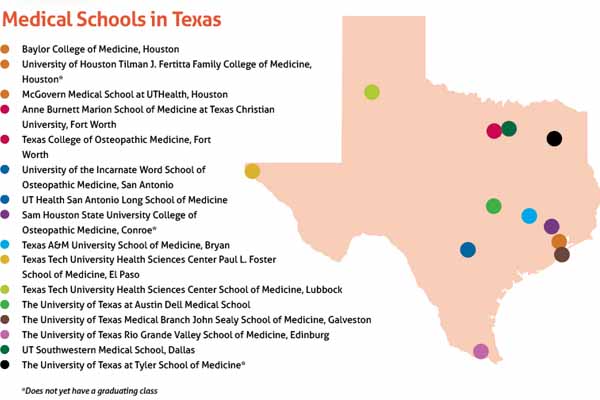
UTRGV is one of seven new Texas medical schools launched since 2016, bringing the total number in the state to 16. The newest, The University of Texas at Tyler School of Medicine, will hold its first classes in July. (See “Medical Schools in Texas,” page 41.)
About 50% of UTGRV’s 2023 medical graduates are staying in Texas – similar to national figures – while the rest went to 11 other states.
Keeping Texas medical students in the state for residency is a top goal for the Texas Medical Association because research shows residents tend to stay and set up practice where they train. About 80% of in-state Texas medical residents stay and practice here, according to the Texas Higher Education Coordinating Board.
All of those physicians are needed to offset a large and growing shortage in the profession. Despite having 8.8% of the U.S. population, the state has 7.3% of active U.S. physicians, according to data collected by TMA. And Texas’ ratio of 204.6 patient care physicians per 100,000 people remains below the national average of 247.5.
TMA has spearheaded successful efforts to expand the state’s residency programs not only to keep pace with the growth in medical schools but also to make sure the state has enough physicians to care for Texas’ exploding population.
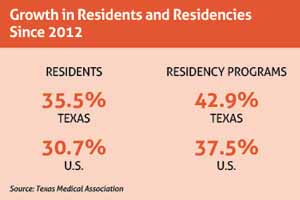
TMA-backed legislation has helped create more than 465 first-year residency slots since 2014 through state grants to help keep Texas medical school graduates in Texas. TMA also is pushing in this year’s session of the Texas Legislature for increased funding for graduate medical education, loan forgiveness, and rural training programs that could help bring more physicians to the state. (See “Growth in Residents and Residencies Since 2012,” below.)
It’s hard to overstate the impact COVID-19 had on the experience of this group of medical students, Mr. Benitez says.
“It was definitely a drastic change for everyone – from things going virtual to everyone isolating and being isolated from the rest of your class ... and your professors,” he said.
Those types of crisis reactions to COVID-19 have obviously tapered off and medical school life more closely resembles pre-pandemic life, Dr. Vela says.
But vestiges of COVID remain, including the fact that all resident interviews for this Match were done online – something unthinkable before COVID-19. Virtually all 2023-24 residency interviews will be online as well, according to the Association of American Medical Colleges.
Because of the pandemic, this class wasn’t able to spend as much time together as most medical school classes, says fourth-year student Saba Suleman, who matched for a transitional residency year at Baylor Scott & White All Saints Medical Center in Fort Worth and plans to pivot after that to dermatology.
“As the pandemic started dying down and we started going back to in-person events, we really started to value each other’s company,” she said. “Any moment we were able to get together was a moment we will want to keepsake forever.”
Even in the best of times, matching right away is not a given for all medical students. In 2022, the year with the most recent data available for Texas, 93.2% of fourth-year medical students matched initially, and all but 1.4% (27) of the others found a residency in the Supplemental Offer and Acceptance Program.

On the Monday before Match Day, medical students get an email from NRMP telling them if they have matched or not. For those who do match, the Friday ceremony tells them to which specialty program and where.
The Monday email cuts down some on the anxiousness of Match Day, says fourth-year student Ruth Escalera. But waiting to open that envelope was still anxiety-inducing because she could have ended up in one of several states between California and Missouri.
Happily, she landed an obstetrics-gynecology residency in El Paso at Texas Tech University Health Sciences Center – one of her top choices. In time, she hopes that will help her work with women in the lower Rio Grande Valley who struggle to get the maternal medical services they need.
“Now more than ever, people need doctors to advocate for them and practice evidence-based medicine,” she said. “Particularly in the Rio Grande Valley, which is an underserved area with one of the highest poverty levels in the country, people already face insurmountable obstacles to get their health care needs.”
Fourth-year student Sabrina Orta was among the UTRGV students headed out of state, matching to a pediatrics residency at Vanderbilt University Medical Center in Nashville, Tenn., her first choice.
“It’s a big change, but I was influenced by some of my mentors that I have to branch out and get out of my comfort zone a little bit and see different patient demographics, which I think would be really good for me,” she said.
While the residency will take her away from her family in the Houston area, her goal is to return there for a fellowship and then set up a practice.