Thanks to the COVID-19 pandemic, a growing number of public health officials in Texas have their minds in the sewer.
That’s a good thing because wastewater turns out to be a helpful medium for tracking the progress of many infectious diseases.
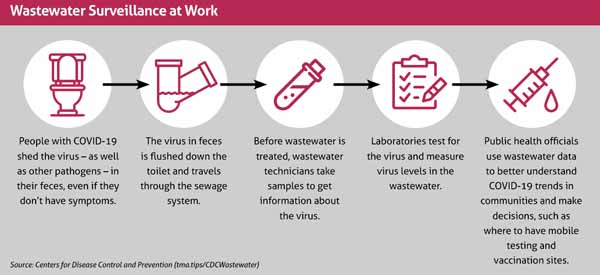
Wastewater-based epidemiology has been around for about two decades, and the principle behind it is simple: Human bodies shed the genetic material of some viruses in waste, and that material accumulates in a region’s wastewater. Sampling the wastewater can tell you if an infection is present and how prevalent it might be. (See “Wastewater Surveillance at Work,” page 45.)
But this type of disease monitoring didn’t take off in Texas and most of the U.S. until early 2020, when the COVID-19 pandemic got underway, according to the Centers for Disease Control and Prevention (CDC).
Especially early in the pandemic, public health officials had few ways to track the novel SARS-CoV-2 virus that causes COVID because people were afraid to visit their physicians to report cases and testing frequently was not available. Public health needed additional tools to monitor COVID, and wastewater turned out to be an effective way to predict when it appeared in a population, in part because it doesn’t require patients to report that they’re sick.
The Houston Health Department – working with Baylor College of Medicine and Rice University – rapidly developed the state’s most comprehensive wastewater surveillance system, and it paid off for local physicians and health care professionals, says David Persse, MD, the health authority for the city of Houston. He compared the experience to building a car as you drive it. But the process was worth the effort because wastewater testing gives far more advance warning than other types of disease monitoring.
“It took us a while to realize that changes in the wastewater value [of SARS-CoV-2] predicted what would happen with our [COVID] positivity rates, and then about two weeks [later] we saw changes in our hospitalization rates,” Dr. Persse said. “So, we didn’t know that wastewater was going to be such a leading indicator.”
Combining that information with other surveillance data, Houston was able to accurately tell hospitals and local physicians when to predict COVID waves.
“Remember at the beginning [of the pandemic], hospitals were just overwhelmed,” Dr. Persse said. “[Hospitals] were trying to balance the elective admissions with the emergency admissions, and the emergency admissions skyrocketed with all these people who were sick with COVID. … So [the wastewater data] gave them an opportunity to adjust their workflows.”
The wastewater data also made it much easier to promote COVID vaccines – once they became available – because it was objective, scientific evidence that case counts were about to rise and that people needed to protect themselves, Dr. Persse says. Unlike surveillance techniques that require reporting by patients and health care professionals, the data are not subjective.
“People were accusing us of being Chicken Little [about potential COVID spikes] all the time, and we could say we have evidence that we’re at the beginning of another wave,” he said.
The wastewater data also showed how effective vaccines were in stopping COVID. Each new variant created a steeper wave in cases – until vaccines came along.
“The slope of increase of the omicron wave, for example, was not as steep as the delta wave,” he said. “And that’s probably because by that time we had a fair number of people vaccinated. So, in retrospect, we’re getting to learn about the phenomena of pandemics.”
Houston’s pioneering efforts made it one of only two cities to earn a “center of excellence” award from CDC.
But other Texas cities and towns used wastewater monitoring to combat COVID as well, and the state has begun building a network of surveillance sites, says infectious disease expert Jennifer Shuford, MD, interim commissioner of the Texas Department of State Health Services (DSHS). The pandemic also prompted CDC to create the National Wastewater Surveillance System, which is independent of the DSHS system (tma.tips/NWSS).
COVID-19 opened up federal funds that allowed local entities to begin wastewater testing, Dr. Shuford says. The DSHS testing network now includes municipal water plants in Waco and Denton as well as some universities, long-term care facilities, and correctional facilities.
Houston’s program tests 168 samples taken from dozens of locations in the Houston area and can report results down to each ZIP code. While some other major metropolitan areas in Texas might need that kind of extensive testing, most communities probably don’t, Dr. Shuford says.
“Houston is a really populous area, so in order to figure out what’s going on in different parts of Houston, you would need to do intensive sampling,” she said. “That might not be true of other communities across Texas that are less populous.”
Wastewater surveillance is so new – and requires the cooperation of so many local entities with varying testing capabilities – that the outlines of a final statewide network remain unclear, Dr. Shuford says. However, it might look like DSHS’s disease testing of mosquitos, in which local entities collect samples and send them to the agency for analysis and public explanation.
DSHS plans to expand its wastewater monitoring system, and not just geographically, Dr. Shuford adds. Some sites in the DSHS network anticipate testing for monkeypox soon, and other diseases, such as polio, are being discussed. Wastewater testing for polio in New York state recently uncovered a previously unknown outbreak. (See “Talk To Your Patients About: The New York Polio Outbreak,” November 2022 Texas Medicine, page 48, www.texmed.org/NYpolio.)
Wastewater surveillance can help track other public health threats as well. For instance, it can be used to identify antimicrobial resistance, which causes about 2.8 million infections and 35,000 deaths in the U.S. each year, according to CDC. This type of surveillance also can be used to track opioid and illicit drug use; levels of caffeine, nicotine, and alcohol consumption; and the presence of pesticides, industrial pollutants, and other environmental toxins.
However, creating a wastewater testing system required overcoming three major hurdles, says Loren Hopkins, PhD, the chief environmental science officer at the Houston Health Department who oversaw the creation of the city’s surveillance system. Those were figuring out how to sample the water, how to analyze the water to get accurate results, and how to use those accurate data once you have them.
The urgency of tracking COVID-19 helped create answers quickly, Dr. Hopkins says. For instance, to ensure accuracy in analyzing the wastewater, she sent identical samples to Baylor College of Medicine and Rice University. Houston Health Department compared the results to identify discrepancies and refine the process.
“We spend hours and hours on the phone talking with each other, going over the data trying to figure out what was the best method for each step in the workflow,” she said.
Now Houston Health Department tests for COVID, flu, and monkeypox, and other diseases – like polio – will be added soon, Dr. Hopkins says. The health department briefs people like the mayor and entities that might be directly affected by the testing results. For instance, the nurse at a school with rising COVID rates would get a heads-up to prepare.
At the same time, the department puts all surveillance information on its website for anyone to see (tma.tips/HoustonWastewater). That information clearly shows who has COVID at a given time – including those who refuse to get tested, those who test at home, and those who are sick but show no symptoms, Dr. Hopkins says.
“It’s passive and its unbiased and reliable,” she said. “Those are the most amazing things about it.”
Houston’s know-how about wastewater surveillance is now being studied in other cities, Dr. Persse says.
“There are many, many communities across the nation that are doing this,” he said.
Texas physicians should be excited by the possibilities of wastewater testing, says Dallas infectious disease specialist Trish Perl, MD, a member of the Texas Medical Association’s COVID-19 Task Force
“My guess is that almost every doctor in TMA would have loved it if they’d had … noticed [early in the pandemic] that – you know what – in two weeks it’s going to be bad,” she said.
That kind of robust public health infrastructure will be especially important as funding for COVID-19 winds down and physicians prepare for the next disease outbreak or pandemic.
“One of the things that happened with COVID is that we saw a lot of pressure on the health care system,” she said. “So, we really need to have these supplemental strategies to give our patients, physicians, health care systems, and emergency planners the best information at any time.”