Right Care, Right Person, Right Time, Right Place
No one worries about the spiraling cost of health care in the United States more than physicians. Our current health care delivery system does too little to coordinate care for patients with expensive-to-manage chronic conditions. Government and other payers are requiring physicians to invest in high-dollar health information technology (HIT) systems without ensuring that the investment translates into better patient care. We are responding to calls to measure a physician’s effectiveness and efficiency, but government metrics imposed on physicians often are off-target. The way to save money in health care is not through ill-advised, random rationing of care, but rather through systems that ensure the right professionals provide the right care, at the right place, and at the right time.
Support physician-driven health care quality initiatives
Physicians are central to ensuring the provision of high-quality, effective, and efficient health care in Texas. The very notion of providing high-quality care is a fundamental principle of physician training, professionalism, and culture.
Today, the term “quality care” has taken on different meanings depending upon which stakeholder is discussing it — a health care policy expert, insurance company CEO, managed care organization executive, patient, or physician. Simply stated, quality is about ensuring the right care is delivered at the right time by the right health care professionals. Unfortunately, our complex health care system, government regulations, and red tape make it increasingly more difficult to provide continuous and consistent care coordination.
Research has shown that quality in our U.S. health care system needs improvement. For example, a 2003 RAND study found many adults received recommended health care services only 55 percent of the time.[20] Misuse, underuse, and overuse of care are the three main areas that can result in patient harm and poor health care quality. With this knowledge, numerous quality improvement initiatives are under way throughout the U.S. health care system.
Physicians are actively striving to improve the quality of care they provide and promote health care innovations that lead to achieving the Triple Aim — better care, better health, and lower costs.

TMA is one of five state medical associations chosen to participate in the American Board of Internal Medicine (ABIM) Foundation’s Choosing Wisely® campaign. Since April 2012, around 60 national medical specialty societies have developed lists of “Things Physicians and Patients Should Question.” The lists are science-based recommendations that physicians have developed and vetted. The Choosing Wisely lists now include more than 300 recommendations regarding treatments, tests, and procedures that national medical specialty societies say are unnecessary or overused. TMA is helping physicians incorporate the program into daily practice.
Already, the Texas Institute of Health Care Quality and Efficiency recommended Choosing Wisely to the Texas Legislature for advancing the state’s version of health care reform passed in 2011. Choosing Wisely dovetails with one of the key values the institute is charged with upholding — making sure state quality initiatives are based on solid scientific evidence.
“When the American Academy of Neurology released their tips, I printed the suggestions out and taped them to my desk as a reminder.”
— Eddie Patton, MD, a Houston neurologist, uses the Choosing Wisely guidelines in his practice.
Promote the patient-centered medical home for every Texan
Consider that the costliest 1 percent of patients in the United State account for more than 20 percent of the nation’s health care spending. They are older patients with cancer, diabetes, heart disease, and other serious and chronic conditions. Many have multiple health problems and may not have relatives who can help with their care.
As public and private payers look for ways to reduce costs, improve patient outcomes, and ease barriers to access, they are turning to models of care that increase economic efficiencies and enhance patient care. One of these is the patient-centered medical home (PCMH). A PCMH is a primary care physician or physician-led team who ensures that patient care is assessable, coordinated, comprehensive, patient-centered, and culturally relevant. The physician or team directly provides, coordinates, or arranges health care or social support services as indicated by the patient’s individual medical needs and the best available medical evidence. The model uses a team-based approach, with the patient’s primary care physician leading the coordination of care. Trained teams and well-constructed electronic health records are keys to a successful PCMH.
TMA supports the use of the PCMH model in Medicare, Texas Medicaid, and commercial insurance plans. Given the budget constraints Texas faces and a growing population with unique health care needs, the PCMH offers the potential for Medicaid cost savings as well as improved patient outcomes and physician and provider satisfaction.
In recent years, numerous states have implemented PCMH initiatives that engage both private and public payers. While each program design was unique and each measured success differently, the evidence indicates the model improves outcomes and reduces costs.
• The Patient-Centered Primary Care Collaborative published a literature review in January 2014. The authors reviewed 20 academic and industry-funded studies assessing how the PCMH model affected patient care, costs, utilization, and quality. According to the report, when primary care practices embrace the model, there are positive outcomes. Specifically, the literature review found that the PCMH:
° Decreases the cost of care;
° Reduces unnecessary or avoidable emergency department services, and hospital admissions and readmissions; and
° Increases preventive health services, such as cancer screenings and immunizations.[21]
• A March 2014 study published in the American Journal of Managed Care found that the PCMH model “significantly reduced costs and utilization for the highest-risk [non-pediatric] patients” by decreasing inpatient hospital admissions.[22]
Texas lawmakers have embraced the idea. In 2009, they directed Texas Medicaid to work with Medicaid HMOs to expand the PCMH model; they directed the Employee Retirement System (ERS) to test it for state employees in 2011. ERS implemented its first PCMH pilot in Austin. The model has been expanded to additional clinics in Houston, Tyler, and Lubbock that collectively cover more than 52,000 state employees. According to ERS, the PCMH has saved the system $31 million since 2011 by reducing inappropriate emergency department visits and hospital readmissions.
A number of Medicaid HMOs, including Driscoll Children’s Health Plan and Texas Children’s Health Plan, are collaborating with physicians to implement the PCMH model in their networks.
In 2013, the legislature enacted a pilot pregnancy medical home for Medicaid enrollees in Houston. It is one of many outcomes-based initiatives Texas is testing to improve maternal and infant health. The pregnancy medical home pilot, led by a team of physicians in collaboration with certified nurse midwives, social workers, and other providers, integrates medical and social support services into a single location to improve the quality of care provided to pregnant women and their children. The results of the Texas pilot will be published in early 2015.
North Carolina, which initiated a similar pilot in 2011, has seen positive results. The state achieved a 3-percent reduction in low-birth weight babies as well as modest declines in cesarean deliveries. Furthermore, the North Carolina pilot increased patient access to comprehensive medical care, resulting in more women receiving health screenings to identify factors that may lead to premature delivery, such as smoking or a prior preterm birth.[23]
Promote physician-led health care teams
Texas needs more physicians and other health care professionals working in all parts of the state, especially in rural and border Texas. But the real gains in improving access to and coordination of patient care will come largely from solidifying and expanding the use of physician-led teams. Team-based care capitalizes on the efficiencies of having the right professional providing the right services to the right patient at the right time … with overall direction and coordination in the hands of physicians.
In 2013, lawmakers bolstered this model by passing legislation that set up a more collaborative, delegated practice among physicians and advanced practice registered nurses (APRNs) or physician assistants (PAs). The new law reinforces the importance of physician-led medical care teams, recognizes the skills all practitioners bring to patient care, and allows the delegating/supervising physician greater flexibility to improve access to care and maintain quality of care. The new law recognizes that independent diagnosis and prescribing are the practice of medicine. Physicians may delegate, but they must supervise.
TMA believes that a physician-led team approach to care, with each member of the health care team providing care based on his or her education and training, is critical to ensuring that more Texans receive high-quality care. Team care requires cooperation and collaboration among all professionals, with a focus on quality, measureable outcomes, and efficient utilization of resources.
A small number of allied health professionals have spurred calls for Texas to grant them independent practice. Such an expansion in their scope of practice would likely increase costs and utilization, and could endanger the safety of our patients. The Texas Medical Practice Act was passed more than 130 years ago to protect Texans from people who called themselves “doctor” but who did not have the skills, training, or education to warrant such a title. The act, administered by the Texas Medical Board (TMB), clearly defines the practice of medicine and the educational qualifications necessary to diagnose, independently prescribe, and direct patient care — and to be held accountable for that care.
In the coming decade, integrating the talents of a diverse medical team under physician leadership will be one of the key challenges. Without physician direction, supervision, management, and coordination, medical care will trend toward even more fractured care, higher-than-necessary utilization, and creeping inefficiencies. This will lead to even higher costs, duplications of services, and lower-quality patient care. These inefficiencies in turn will hamper efforts to improve access to care.
On the other hand, some scope expansions are consistent with team care, are based on objective educational standards, and would improve patient care services. These should be carefully weighed and likely will involve regulatory oversight by TMB.
Improve health care coverage for low-income Texans
The Affordable Care Act (ACA) created two coverage options for uninsured patients with incomes up to 400 percent of the federal poverty level (FPL). One choice, which the U.S. Supreme Court made optional for states, was expanding Medicaid eligibility to 138 percent of FPL ($16,104 for an individual or $32,913 for a family of four in 2014).[
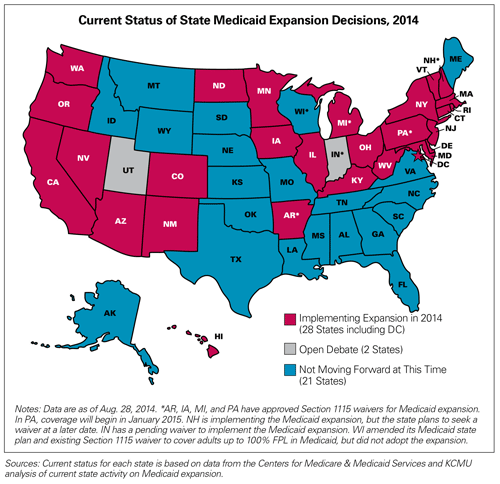
24] The other was the new health insurance marketplaces, where patients go to buy private insurance. Texas is one of 21 states that chose not to expand Medicaid eligibility in 2014. As a result, more than 1 million uninsured Texans, mostly low-income adults, are left in what’s called the “coverage gap,” which means they make too much money to qualify for Texas Medicaid but not enough to qualify for the marketplace premium tax credits. Few of these Texans have access to other affordable insurance options. Texas Medicaid eligibility for parents is about 20 percent of poverty — less than $4,000 per year.
Most of these Texans work. In fact, 58 percent, more than 845,000, are currently working or have worked within the past year. Of the 42 percent who are not working, a majority (24 percent of Texans who could gain coverage under the coverage gap) are classified as “not in the workforce.” They include people with disabilities, college students, non-working spouses who care for children or a family member with a disability, and people who have left the workforce. The remaining 18 percent of Texans who could be helped are unemployed.[25] Although they work, few in the coverage gap have access to employer-sponsored coverage; if they do, they frequently forego coverage because of high costs.
Texas physicians want to ensure all Texans have access to coverage and, more important, have access to physicians and other health care providers. According to the Institute of Medicine, even when uninsured patients have access to safety net services, the lack of health insurance often results in delayed diagnoses and treatment of chronic diseases or injuries, needless suffering, and even death.
That’s why TMA supports allowing state leaders to work with the Centers for Medicare & Medicaid Services (CMS) to develop a comprehensive solution that fits Texas’ unique health care needs. Several states have taken this step with some success, including Indiana, Arkansas, Iowa, Michigan, and Pennsylvania. (See adjacent chart.) TMA believes the Texas Legislature too can create an ingenious solution that works for the state and helps Texans in the coverage gap get affordable and timely care. Any Texas-style solution expanding access must:
- Draw down all available federal dollars to expand access to health care for poor Texans;
- Give Texas the flexibility to change the plan as our needs and circumstances change;
- Clear away Medicaid’s financial, administrative, and regulatory hurdles that are driving up costs and driving Texas physicians away from the program;
- Relieve local Texas taxpayers and Texans with insurance from the unfair and unnecessary burden of paying the entire cost of caring for their uninsured neighbors;
- Provide Medicaid payments directly to physicians at least equal to those of Medicare payments; and
- Continue to improve due process of law for physicians and other providers in Texas as it relates to the Office of Inspector General.

Improve maternal and infant health
The March of Dimes gave Texas a “C” on its prematurity report card in 2013. The Texas Health and Human Services Commission reported 67 percent of hospital costs for newborns is for prematurity. Neonatal intensive care for an extremely preterm birth costs Medicaid an average of $54,400 versus $480 for a full-term baby. Babies born prematurely often suffer from chronic illnesses, such as asthma, and developmental delays or learning disabilities, all of which further increase health care costs as well as costs to the state’s educational system. According to the Centers for Disease Control and Prevention (CDC), the leading cause of neurological disability in children is prematurity.
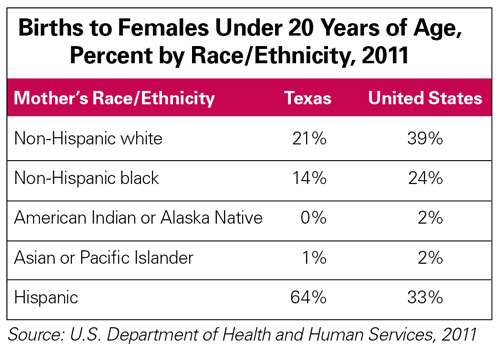
Improving birth outcomes not only enhances the lives of babies, mothers, and their families, but also can yield substantial savings, particularly to publicly financed programs such as Medicaid, which covers 53 percent of all Texas births.
Almost 60 percent of Texas women lack health insurance. Roughly 700,000 of these women are in the so-called “coverage gap” — earning too much for Medicaid (unless they are pregnant) but too little to qualify for subsidies to help buy private insurance on the federal exchange.
Without coverage, uninsured women often forego needed care, particularly preventive care. Preventive health services are important for all patients, but especially for women, who require prenatal care during pregnancy and other types of preventive care, such as cancer screenings, high blood pressure checks, nutrition counseling, and birth control before and between pregnancies to ensure they and their babies are healthy.
Texas has three programs that collectively serve as the preventive health safety net for low-income women — Texas Women’s Health Program (TWHP), Expanded Primary Health Care Program (EPHC), and family planning initiatives. Texas has the capacity to serve only about one-quarter of the women who qualify for these programs.
Reduce Texas' maternal mortality rates Texas statistics for maternal mortality more closely resemble a third-world country than a state with world-class medical care. About 12.3 percent of babies are born prematurely — higher than the U.S. rate of 11.7. Rates are highest among African- American women. The national goal is 9.6 percent by 2020.
Factors that contribute to poor maternal and infant health are lack of early prenatal care, diabetes, hypertension, and obesity. Too many Texas women must confront some or all of these challenges.
Texas has made progress in the past two legislative sessions improving outcomes on maternal illnesses and deaths. In 2011, the Texas Department of State Health Services (DSHS) and the March of Dimes launched the Healthy Texas Babies Initiative (HTBI), bringing together health and community leaders to develop state and local strategies to address Texas’ poor maternal and birth outcomes. Texas Medicaid, with strong support from TMA and the state’s two OB-Gyn specialty societies, implemented 2011 legislation to halt payment for non-medically necessary, elective inductions prior to the 39th week of gestation. The 2013 legislature established a Maternal Mortality and Morbidity Review Task Force to identify causes of and remedies for pregnancy-related deaths and severe morbidity. Lawmakers also reversed funding cuts enacted in 2011 to DSHS-administered women’s preventive health care, which left more than 200,000 women without access to these vital services.
More work remains. Increasing the number of women who enroll in the Texas Women’s Health Program, EPHC, and family planning programs, as well as increasing the number of physicians and clinics who participate, will be essential to Texas’ efforts to improve maternal health and birth outcomes.
Improve patient access to safe health care: Telemedicine
Texas has one of the fastest growing populations in the United States. This dramatic growth necessitates a robust health care workforce across the state. Currently, 32 Texas counties have no practicing physician. Some areas of the state have critical shortages of specialists. Physicians need tools such as telemedicine that can provide safe, high-quality, timely care to patients. Physicians, patients, and lawmakers should examine how to make telemedicine an effective tool that will improve access, decrease health care costs, and improve patient health. However, we must maintain safeguards to protect patients and ensure telemedicine complements the efforts of local health care providers.
Good telemedicine standard of care
TMA has long-standing policy — first adopted in the 1990s — in support of physicians and providers rendering safe, high-quality telemedical services. TMB amended its telemedicine rules in 2010 to ensure medical services delivered this way observe the same standards of care as traditional medicine. Those rules, developed with input and support from TMA, academic health science centers, and health technology companies, require an established patient-physician relationship and state that an online or telephonic evaluation solely by questionnaire does not constitute an acceptable standard of care. A patient-physician relationship must begin with an initial face-to-face visit; a relationship cannot be established solely by a phone call, online questionnaire, or Internet “face-time” discussion.
If a traditional patient visit requires a physical examination of the patient, that same standard will apply to a telemedical visit. That is why a true telemedical service requires a local observer or presenter to perform the necessary physical non-virtual examination. Merely filling out a questionnaire or speaking over the phone provides subjective information only and can lead to incorrect diagnosis and treatment.
In the 2011 and 2013 legislative sessions, for-profit telemedicine and insurance companies pushed legislation that would allow them to provide telemedicine services in Texas without an established patient-physician relationship. Their efforts failed, but they are likely to try again in 2015. Their efforts thus far have focused solely on getting the health plan enrollees to pay more out of pocket for a telemedicine transaction, as the health plan pays nothing for the service. TMA will continue to protect patient safety by ensuring anyone who provides telemedicine does so under TMB rules.
TMA strongly supports TMB’s telemedicine rule regarding the initial face-to-face visit, the recognition of local coverage arrangements, and the necessity for an observer (licensed health care practitioner) for all new medical conditions. TMA will continue to fight for safe medical care delivery and oppose business models that do not meet appropriate standards of care.
Ensure equal pay and follow-up for after-hours care
Insurance companies generally don’t pay physicians for the time they spend with patients over the telephone for after-hours care. TMA supports legislation that will allow physicians to bill patients for after-hours telephone consultations. This parity is critical to ensure patients can maintain continuity of care with their physician. Also, when telemedicine services are provided to patients, the telemedicine company needs to make certain that all treatment provided is communicated to the patient’s local physicians to guarantee appropriate continuity of care or in case the patient needs follow-up care.
They are worth his patients’ very lives. “[Using telemedicine] we have the opportunity to create all sorts of innovative engagements with patients on the remote end for the betterment of their care, to take care of at-risk populations who aren’t cared for at all or so minimally that it costs everyone,” says Dr. Kim. But the first step, he says, “is to establish a therapeutic relationship. To do that, I need a picture, and I need sound. Without both, I do not know how I would be able to render an assessment, opinion, or recommendation, including … and especially … the prescribing of medications. In my opinion, this is the minimum bar for telehealth care.”
— To Thomas J. Kim, MD, pictures are worth more than a thousand words
Current barriers to telemedicine services
Interstate licensing compact: Because telemedicine programs involve physicians treating patients remotely and often across state lines, physicians using telemedicine technology must comply with each state’s licensing requirements. Recently, the Federation of State Medical Boards (FSMB) proposed an interstate medical licensure compact that would allow physicians to practice telemedicine in multiple states without having to go through each state’s individual licensure application process. State boards would mutually agree to a common set of requirements to help streamline licensing and greatly reduce the hassle of a full licensure application evaluation. TMB recently decided to move forward on discussing the proposal.
Expedited credentialing: In 2011, CMS and the Joint Commission promulgated rules allowing hospitals using telemedicine to rely on credentialing conducted at the facility where the physician is located. However, some physicians report hospitals still frequently require complete credentialing, even when doctors in another geographic location deliver services only via telemedicine. TMA and the Texas Hospital Association are working with HHSC’s Quality-Based Payment Advisory Committee to develop a uniform approach to telemedicine credentialing in line with CMS and Joint Commission regulations and state rules.
A typical telemedical visit is conducted with a physician at a remote location using video and audio to connect to a patient who is accompanied by a licensed health care provider (acting as the local observer for the physician). The observer is able to take objective measurements, such as blood pressure, heart rate, and weight, that the physician needs to provide treatment safely.

- Advocate for the patient-centered medical home (PCMH) model and financial incentives from both state and private payers. Recognize the significant start-up costs for transforming a typical primary care, fee-for-service practice into a fully functional medical home.
- Support legislation allowing state leaders to work with the Centers for Medicare & Medicaid Services (CMS) in developing a comprehensive coverage solution for the unique health care needs of Texas.
- Institute incentives for physicians who find innovative solutions to save Medicaid costs without increasing the overall cost of care.
- Stop any efforts to expand scope of practice beyond that safely permitted by nonphysician practitioners’ education, training, and skills.
- Enact only those changes to scope of practice laws that are based on objective educational standards, improve patient care services, protect patient safety, preserve the physician-led medical home, are consistent with team care, and have appropriate regulatory oversight by the Texas Medical Board (TMB).
- Pass legislation that strengthens TMB’s regulatory oversight of nonphysician licensees who, by specific educational achievement, are granted authority to perform acts traditionally reserved for and defined as the practice of medicine.
- Increase funding for women’s preventive health services to ensure all women in need can obtain services.
- Evaluate efficacy of Texas Health and Human Services Commission (HHSC) and Department of State Health Services (DSHS) patient, physician, and provider outreach for women’s health programs as well as whether state-funded programs have sufficient physician and provider capacity.
- Continue collaborative, evidence-based efforts with physicians and other stakeholders that will reduce preventable preterm births, including implementing measures to ensure uninsured, low-income women have timely access to appropriate early preventive health care before, during, and between pregnancies.
- Intensify smoking cessation efforts for pregnant women.
- Support implementation of neonatal intensive care and maternal standards of care, both of which the HHSC Perinatal Advisory Council is developing.
- Ensure adequate resources for the Maternal Mortality and Morbidity Review Task Force as well as the Fetal, Infant, and Child Mortality Review Program.
- Identify the population of pregnant women at higher risk of a poor birth outcome due to abuse of alcohol, opioids, or other substance, and amplify educational and outreach efforts to physicians and patients regarding Medicaid substance abuse treatment resources.
- Invest funding in research to identify genetic, economic, and social factors contributing to higher rates of preterm births.
- Ensure telemedicine services are provided in accordance with TMB rules and accepted standards of care.
- Enact legislation that would require insurance companies to pay local physicians for after-hours telephone and telemedical consultations on the same basis as other physicians who may be working for a telemedical business and permit them to contract with patients for this added service.
- Require any telemedical service to be communicated to the patient’s local physician to ensure continuity of care.
- Support an interstate compact for telemedicine licensing that ensures state sovereignty over the practice of medicine.
- Allow expedited credentialing at hospitals for distant-site physicians who provide telemedicine services to the facility.
Healthy Vision 2020