Texas has a large, diverse, and growing population that is growing less healthy and more ethnically diverse, and needs more and better-coordinated health care services.
Unfortunately, Texas — compared to other parts of the country — has significant shortages in most physician specialties and other health care professionals.[1] Although our 2003 liability reforms have helped to establish Texas as a good place to practice medicine and we have record numbers of physicians applying for licensure, the current supply won’t keep up with the demand. Texas has unique challenges, with some of the nation’s largest urban centers as well as the vast expanses of sparsely populated rural regions. We need to invest more in our medical schools and graduate medical education (GME) training programs. With the numerous shortages, we must focus on building physician-led teams that can safely meet the diverse and complex health care needs of the Texas population.
Meet the growing demand for medical care with clinically appropriate medical services
Texas’ population is expected to boom from 25 million to almost 45 million by 2040.[2] This means not only more people who need medical care, but also a larger demand for more health care services from a growing populace of increasingly obese Texans and the generally sicker elderly residents.
Texas has long been challenged to produce or recruit enough physicians to keep up with our rapidly growing population. The sheer size of the state’s population is the biggest driver of physician demand. The state’s broad expanse and varied geography and demographics, plus the great attraction for others to move to Texas, result in an ever-increasing demand for physicians and other health care professionals. Over the past two decades, Texas has led the country in population growth.[3]
The convergence of a larger, increasingly aging, and increasingly obese population of Texans represents “a recipe for disaster.” In the United States, approximately 80 percent of all persons 65 and older have at least one chronic condition, and half have at least two.[4] These patients take longer to treat, and the amount of services and care they require grows more and more complex. Diabetes, which causes excess morbidity, premature mortality, and increased health care costs, affects about 1.8 million adult Texans.[5]
As adults live longer, the prevalence of Alzheimer’s disease also increases. An estimated 13 percent of those age 65 and older have Alzheimer’s. The number doubles as people reach 85 and older. In Texas, about 340,000 Texans suffer from the disease.[6]
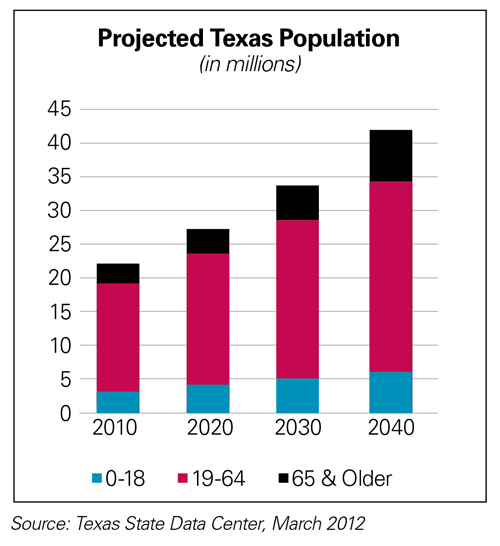
Texas is a state with significant shortages of physicians and other health care professionals. Several powerful trends are pushing those shortages to levels that will further threaten Texans’ ability to access care, regardless of where they live or whether they have health insurance coverage. In addition to Texas’ ethnic diversity and 1,254-mile shared border with Mexico, those trends include:
- High population growth: Texas added 8 million residents from 1990 to 2010 and is expected to add another 5 million by 2020;[7]
- More seniors: By 2020, more than 5.7 million Texas baby boomers become eligible for Medicare, the age group with the highest demand for primary and specialty care physician services;[8]
- High birth rate: Texas has the third-highest birth rate in the nation, increasing demand for obstetrical, pediatric, and neonatal physician services;[9]
- More chronic disease: Many Texans suffer from chronic diseases such as diabetes and hypertension, which frequently require more health care services; and
- High rates of poverty.
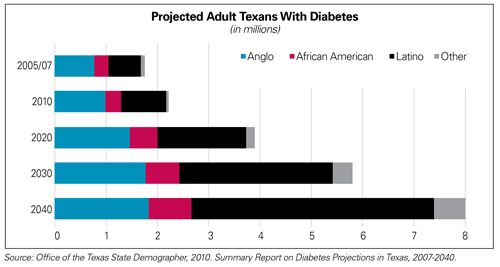
More and more Texans will experience health-related disparities because of poor health status and/or a lack of preventive health options or access to timely medical care. Health disparities include differences in the occurrence or prevalence of a disease or a poor health condition. For example, the Texas Diabetes Council estimates that the number of adult Texans with diabetes will quadruple from the current 1.7 million to almost 8 million in 2040. This surge is strongly associated with population growths in Latinos and African-Americans, who have higher rates of diabetes.
People with diabetes and other chronic health conditions have complex care needs. Their physicians not only must treat the condition itself, but also must lead a team of caregivers who rally all the resources to help prevent health complications and greater health care costs for the patient.
Physicians must be the backbone of such a complex system of care if it is to be high quality and cost-effective. Otherwise, the state’s efforts to increase preventive care, improve medically necessary treatment for the chronically ill, and reduce inappropriate emergency department visits will falter. Physicians also play an important role in developing and partnering with the public health system. This partnership can enhance local coordination of care, disease surveillance, access, and health promotion.
Make sure enough physicians and other health care professionals are working in all parts of Texas
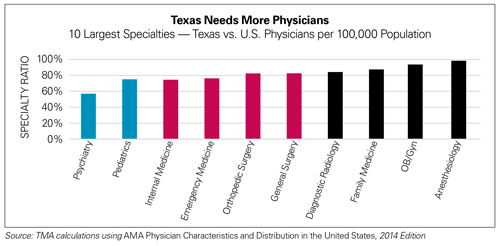
Texas has a shortage of both primary care physicians and other specialists. Texas ranks behind nearly every other state in the number of patient care physicians per capita and usually ranks last among the most populous states.[10] To evaluate this shortage across specialties, we have devised a metric that compares the number of Texas physicians per 100,000 population with the U.S. average by specialty. We call this the “Texas Specialty Ratio.” The closer this ratio is to 100 percent for a given specialty, the closer Texas is to the national average.
- Texas has fewer physicians per capita than the national average for 36 out of 40 major medical specialty groups.
- Psychiatry, preventive medicine, and child/ adolescent psychiatry are among the specialties with the lowest Texas Specialty Ratios.
- The four specialties with higher Texas Specialty Ratios are aerospace medicine, medical genetics, transplant surgery, and colon and rectal surgery.
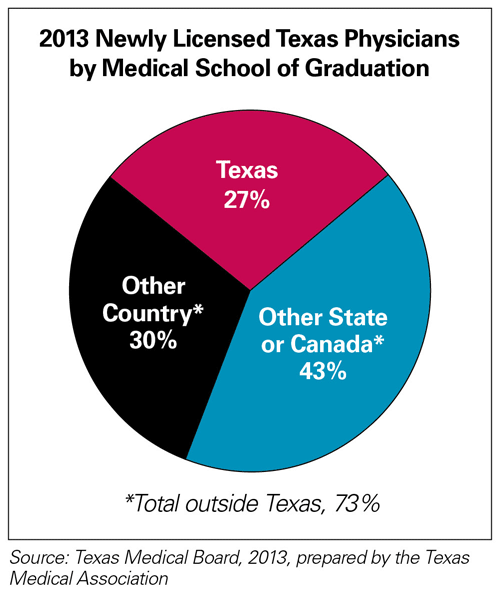
Texas ranks fourth among the six most-populous states in medical students and resident physicians per capita.[11] Despite the ongoing success of our 2003 medical liability reforms, Texas continues to be overly dependent on other states and countries for supplying new physicians. Last year, 73 percent of newly licensed physicians graduated from medical schools outside of Texas.[12]
To meet future physician demands, Texas needs a stable, high-quality medical education system to produce homegrown physicians. We must provide a reasonable opportunity for Texas medical school graduates to obtain their residency training in the state without being forced to leave home. Multiple studies confirm that physicians who complete both medical school and residency training in the state are three times more likely to practice here.[13]
Because the human body is complex, the mastery of medical care is correspondingly complex, requiring a lengthy educational and training pipeline. After college, physicians traditionally complete a four-year medical school education, followed by specialty training in residency programs for three to eight additional years, depending on specialty.
Considering the significant challenges the state faces in meeting its health care workforce needs, state leaders must support a comprehensive health professions workforce analysis that includes all appropriate stakeholders and visualizes the needs of Texas for the short and long term.
Ensure Texas medical school graduates remain in the state for specialty training
Texas is now educating the largest number of medical students in its history.[14] These gains will be lost to us, however, if we do not create sufficient numbers of high-quality, entry-level residency training positions to incentivize these students to remain in the state for specialty training.
Many parts of the United States are in the midst of medical education building campaigns. Texas is among the leaders, having reached the nationally recommended 30-percent growth in medical school enrollments over the past decade. Following establishment of the three medical schools now under development and growth at other schools, the number of graduates is projected to peak at 2,000 by 2022.[15]
In 2013, almost half (49 percent) of Texas medical school graduates left the state for residency training.[16] Texas invests $176,000 in each medical student’s four years of education.[17] Texas physicians are concerned about the state’s ability to protect that growing investment with enough GME positions to meet demand.
For 2013, there were 1,611 entry-level GME positions offered in Texas. By comparison, 1,587 students graduated from Texas medical schools in 2013. The Texas Higher Education Coordinating Board recommends a ratio of 1.1 entry-level GME positions for each Texas medical school graduate. To meet this goal, Texas would have needed 1,746 entry-level training positions in 2013, or 135 additional positions.
Texas needs continued and stable state support for both critical parts of a physician’s education and training to help cultivate future generations of Texas physicians trained to deliver care in the evolving health care delivery systems, ensuring stable access to health care for all Texans.
Texas medical school graduates are projected to peak at 2,000 in 2022. This will mean an even greater demand for residency training positions to enable graduates to remain in the state. To achieve the 1.1-ratio goal after enrollments reach the peak, Texas will need to add 589 GME positions to the 2013 numbers.
Medical education is a public good and a tremendous economic asset to the state
- Academic health centers generate an additional $1.30 in economic activity for every dollar spent.
- Texas ranks fifth among states in the total economic impact of academic health centers. These centers serve as major employers in their communities and impact 210,000 jobs. Many of these are filled by highly educated and skilled workers at higher salary levels.[18]
- Academic health centers have a major financial impact in every region they are located: Houston, Dallas, Bryan/College Station, Temple, Lubbock, El Paso, San Antonio, Fort Worth, and Tyler.
To successfully retain our own medical graduates for residency training and entry into practice, Texas must:
- Have an adequate number of training positions,
- Ensure residency programs have enough resources to provide high-quality training,
- Attract and retain well-qualified faculty,
- Evaluate the impact of the newly established GME expansion grant programs on GME capacity and retention of our medical school graduates for training, and
- Provide incentives for teaching hospitals to create new GME positions and maximize the potential for adding residency teaching at other hospitals that have not previously participated in residency training.
Texas must make sure that our medical school graduates are fully informed of the state’s strong interest in retaining them for training and eventual practice.
Improve rural access to care
Physician shortages constitute a special problem in rural areas of the state. The continued urbanization of Texas exacerbates this long-standing problem. Approximately 12 percent of Texans live in rural counties, yet only 9 percent of primary care physicians practice there. In 2013, Texas had 52.3 primary care physicians per 100,000 population in rural areas versus 73 per 100,000 in urban areas.[19] Physician shortages in rural areas not only hinder access to primary and specialty care, but they also serve as impediments to attracting new businesses to those areas, and ultimately lead to diminished quality of life for residents and years of lost productivity. A number of factors hurt physicians’ ability to open and sustain rural practices, including heavy concentrations of Medicare, Medicaid, and uninsured patients; professional isolation and lack of health care infrastructure; and high debt after medical school.
Physician practices in rural Texas contribute to the local economy in at least four critical ways.
- They employ administrative and clinical staff to help care for patients. On average, a solo primary care physician in a rural area will employ three staff: a registered nurse, a medical technician or licensed vocational nurse, and a receptionist/ billing clerk.
- They contribute revenue to and generate additional employment at local hospitals through inpatient admissions and outpatient services.
- They have a ripple effect on employment and economic activity such as pharmacies; physical, occupational, speech, and inhalation therapy; and medical equipment and device sales.
- They generate essential tax revenues for their communities.
If rural physician practices and rural economies are to survive and thrive, physicians need incentives to practice in those areas, particularly if the state and federal governments fail to provide appropriate payments for Medicaid and Medicare services. Medical school programs with rural-focused curricula and residency training tracks increase the potential supply of primary care doctors in underserved areas as do loan forgiveness programs like the National Health Service Corps and the State’s Physician Education Loan Repayment Program.

- Preserve and protect state support for undergraduate medical education and cultivate the future generation of Texas physicians, thus ensuring stable access to quality health care for all Texans.
- Support and develop new graduate medical education (GME) programs in the specialties that best reflect the state’s health care needs. Support incentives for hospitals and other community-based agencies to develop residency programs in the specialties most needed.
- Direct the Texas Higher Education Coordinating Board to monitor the availability of GME training positions so that Texas can retain our graduates for residency training and beyond.
- Sponsor research that will identify and promote innovations in training family medicine residents for practice in Texas.
- Maintain and build on the current bonus payments for primary care physicians under Medicaid, and extend it to other specialties to ensure medical services are available throughout Texas, particularly in rural areas.
Healthy Vision 2020