Texas physicians strongly support Medicaid. Without it, nearly 4 million poor and low-income Texans would lack health insurance, jeopardizing their health and well-being. Physicians want to take care of these patients, and they do so throughout the state. Unfortunately, red tape and bureaucratic hassles coupled with low pay are forcing many physicians to limit the number of new Medicaid patients they take — or to not take any at all. For more than a decade, physician participation rates have been in a free fall, plummeting 33 points in 14 years. In 2000, 67 percent of Texas physicians reported accepting all new Medicaid patients; today, only 34 percent do.
Physicians don’t reach this decision easily. They want to provide prenatal care to pregnant women, medications for asthmatic children, and community services for seniors wishing to stay in their homes instead of a nursing facility. But after doctors care for a Medicaid patient, their office staff must then navigate the program’s increasingly complex rules and bureaucratic regulations to get paid.
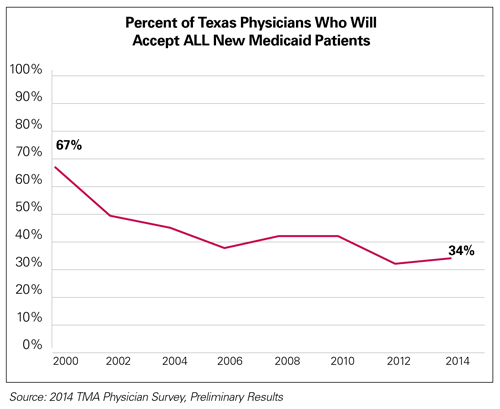
Administrative hassles not only detract from a physician’s ability to provide needed care, they also drive up overhead costs, ultimately making the meager Medicaid payments too low for many physicians to put up with the tangle of red tape.
Standardize Medicaid managed care administrative processes
Federal and state Medicaid laws and regulations are extremely complex. Physicians participating in Medicaid must comply with all of the requirements of the Texas Medicaid Provider Procedures Manual, which exceeds 1,800 pages, as well as all state and federal laws governing or regulating Medicaid. Physicians also must abide by additional requirements imposed by multiple Medicaid HMOs. Pediatricians practicing in Harlingen, for example, must be familiar with traditional Medicaid rules plus five different Medicaid HMO plans if they participate in all six products.
While all Texas Medicaid plans cover the same essential patient benefits and services, what it takes to receive approval to provide the care — or get paid for it — varies with each plan. For instance, one Medicaid HMO may require prior approval for therapy provided to children with disabilities; another may not. Or each Medicaid HMO may require prior approval of the same service, but use different criteria to grant approval.
Many physicians who want to participate in Medicaid have found just signing up for the program daunting. They must complete a confusing application, submit it to the state, then hope their answers are correct because if not, the application is returned. Sometimes physicians’ applications are lost, and they have to redo it. Physicians frequently spend months navigating the state’s application process. Once Medicaid approves the application, physicians then must be credentialed by each Medicaid HMO they agree to contract with, even though the information each plan needs to complete the credentialing process is nearly identical to the original Medicaid application. All these time-consuming administrative issues serve as barriers for physicians who want to take care of Medicaid patients.
Improve Medicaid HMO physician networks
Perhaps the worst hassle of all is contending with inadequate Medicaid HMO physician networks. Contractually, state and federal governments require each plan to have an adequate number of primary care and subspecialty physicians to provide timely care for the patients in their networks. But in practice, this is not always the case. Patients and physicians frequently complain that physicians and providers listed in HMO directories as accepting new Medicaid patients either are not accepting them at all or have excessive wait times for new patient appointments.
Primary care physicians say it is not uncommon to spend hours on the phone trying to find specialty care for a Medicaid patient. Too often, they resort to referring their patients to costly emergency departments to ensure their patients get the care they need.
Significant expansion of these networks will not happen until the government eliminates bureaucratic hassles and increases payment rates.
Simplify compliance with Medicaid fraud and abuse laws
For physicians, learning and complying with the Texas Medicaid Provider Procedures Manual, the Texas Administrative Code, state law, and federal statutes and regulations require a significant amount of time and staff resources. On top of the sheer volume of compliance obligations, physicians also must stay up to date with frequent changes and revisions. If physicians fail to strictly comply with all of Medicaid’s requirements, they face stiff fines, penalties, sanctions, or other enforcement actions. This creates an impossible situation for physicians who want to care for Medicaid patients.
Medicaid administrative simplification progress made
Lawmakers in 2013 heard the plea for Medicaid administrative simplification, directing the Texas Health and Human Services Commission (HHSC) to address physician, provider, and patient complaints regarding Medicaid HMO operations. Two new laws require HHSC to reduce administrative hassles, ensure prompt payment of claims, streamline paperwork and credentialing requirements, and strengthen how Medicaid measures network adequacy.
One law established a workgroup to advise HHSC on creation of a Provider Protection Plan. The plan is required to address:
- Prompt payment of claims;
- Adequate and clearly defined provider network standards;
- Prompt credentialing processes; and
- Establishment of electronic means to submit claims, prior authorization requests, and claims appeals, and to obtain remittance advice and explanation of benefits.
Another new committee — the Statewide Medicaid Managed Care Advisory Committee — will advise HHSC on how best to expand the HMO model to new populations and services over the next several years. The committee, led by a TMA physician, also will identify ways to improve network adequacy, reduce HMO hassles, and increase quality, efficiency, and patient, physician and provider satisfaction.
Medicaid rules should be clear and easy to understand so physicians can dedicate their time, talent, and staff resources to patient care, as opposed to administrative hassles, burdensome audits, and fear of fraud and abuse accusations. While TMA supports efforts to eliminate health care fraud, we also strongly support a fair process to define, detect, and prevent actual fraud. HHSC needs to make improvements that will reduce and streamline its red tape to prevent administrative errors in the first place. When HHSC identifies potential compliance problems (whether through an investigation or audit), steps should be taken to resolve them quickly. First, the problem and applicable standards must be communicated to the physician, so he or she has an opportunity to respond to allegations and, in the event an issue does exist, take corrective action.
Second, when allegations of potential fraud, abuse, and/or any overpayments arise, they should be supported by reliable evidence. Accordingly, investigations concerning the practice of medicine must include the expertise of medical practitioners with appropriate training and experience — particularly for questions of whether a service or treatment was medically necessary.
Third, when issues are accurately identified, they should be resolved in a timely manner, especially when the concerns are based on non-fraudulent violations. Timely resolution of non-fraudulent issues allows physicians to correct identified errors and keep their focus on patient care without the distraction of extensive litigation, looming demands, or nonpayment.
TMA believes the best way to reduce administrative and payment errors is through continued education and outreach from HHSC and Medicaid managed care plans. This step would help eliminate costly errors before they occur, saving physicians and their office staff time and money, and ultimately saving taxpayers money as well.
Physicians should be afforded adequate notice of the alleged issues or violations, calculation of overpayments (including extrapolation methodology), and proposed sanctions or penalties; the applicable timelines for responding to allegations; and the right to offer a meaningful response. If issues cannot be settled informally, physicians should be able to appeal the alleged violation and money in question to an independent third party and have that appeal heard in a timely manner.
Texas laws and regulations should clarify the coordination of responsibilities, authority, and interaction among enforcement agencies. Eliminating redundancy would streamline operations, expedite investigations and recovery efforts, and provide physicians with clarity on the legal authority of each investigative agency and the applicable rules and processes.
Eliminate duplicate Medicaid audits and investigations that waste taxpayers’ money
Physicians participating in Medicaid face audits and/or investigations from an array of state agencies or agency contractors. Duplication and overlap of investigations waste taxpayer money, valuable state resources, and time in Texas Medicaid. Seven different state agencies are involved in Medicaid audits and investigations, including the Office of the Attorney General (made up of the Medicaid Fraud Control Unit and the Civil Medicaid Fraud Division), the HHSC Office of Inspector General, managed care organizations (MCOs), MCO Special Investigative Units, and Recovery Audit Program contractors.
Physicians must know which agency is conducting the investigation, who has the authority to settle or resolve an issue, and whether they are being accused of an administrative violation, civil fraud, or criminal activity. Texas laws and regulations should clarify the coordination of responsibilities, authority, and interaction among enforcement agencies. Eliminating redundancy would streamline operations, expedite investigations and recovery efforts, and provide physicians with clarity on the legal authority of each investigative agency and the applicable rules and processes.
Discard costly and burdensome data reporting programs
For more than a decade, Texas physicians who own ambulatory surgery centers (ASCs) or hospitals have had to collect and report data to the Texas Health Care Information Council (THCIC) that provide little or no benefit to patients. Data reporting laws and their subsequent regulations were intended to help patients make informed health care choices, a laudable goal. However, over the past 20 years, the THCIC data reporting program has failed to do this. It only collects physicians’ billing information, which it turns around and sells to third parties, such as large hospital systems and commercial health insurance plans, who use it for marketing. THCIC has not shared any summary data with physicians so they can improve patient safety or quality outcomes. Plus, THCIC’s data reporting requirements are expensive and time-consuming for physicians and their office staff to meet.

- Establish a centralized credentialing portal so physicians can apply to participate in all the Medicaid HMOs participating in the service area simultaneously.
- Integrate Medicaid/Medicaid HMO application and credentialing processes for physicians applying to the program for the first time.
- Improve coordination of benefits between Medicaid and Medicaid HMOs to prevent recoupment of money from physicians after services were provided in good faith.
- Require Medicaid HMOs to communicate clearly to physicians and patients the process for obtaining services when an in-network physician/provider cannot be found.
- Require the HMOs to establish a dedicated contact person for a physician to call to request assistance in arranging services not available in network.
- Establish a Texas Health and Human Services Commission (HHSC) ombudsman to oversee Medicaid HMO network adequacy, respond to patient and physician complaints, and enact physician recruitment initiatives.
- Establish a division within HHSC dedicated to recruiting new physicians to participate in Medicaid, and/or allow the HMOs to recruit physicians who are not enrolled in Medicaid but whose specialty is needed in the network.
- Monitor HMO network adequacy more stringently. Apply stiffer penalties for plans that fail to maintain adequate networks.
- Require the state to publish in-network and out-of-network utilization trends and data about patient/physician complaints.
- Protect 2013 legislation that improves due process for physicians who are confronted with a Medicaid fraud or overpayment accusation.
- Ensure physicians and providers have a meaningful opportunity to appeal allegations of Medicaid fraud and/or abuse to an independent third party.
- Eliminate redundant efforts and expenditure of state funds, employee time, and other resources involved in investigating alleged violations of Medicaid regulations.
- Ensure Texas laws and regulations clarify the coordination of responsibilities, authority, and interaction among enforcement agencies regarding the Medicaid program.
- Eliminate data collection programs, such as the Texas Health Care Information Council, that don’t provide patients with useful information to make informed health care decisions.
TMA Healthy Vision 2020