In the 19 months since the Texas Child Psychiatry Access Network (CPAN) had been up and running, it’s kept any number of minor problems from becoming major ones, says Steven Pliszka, MD, chair of the department of psychiatry at UT Health San Antonio.
CPAN gives pediatricians and family physicians across Texas free telemedicine-based consultation and training on community psychiatry. A pediatrician or family physician caring for a patient with psychiatric needs can call CPAN and typically get professional advice in minutes.
Dr. Pliszka works at one of 12 regional psychiatric centers, or hubs, that CPAN uses to advise primary care physicians, and he recently helped a pediatrician treat a boy in foster care.
The boy, who was being treated for serious behavioral health problems, had recently moved to a new placement, away from his usual psychiatrist. The boy’s new foster parent turned to the pediatrician to keep from running out of medication. The pediatrician
in turn called CPAN and spoke with Dr. Pliszka.
“[The boy was on a] very intensive regime and though entirely within the standard of care, it was not something that a pediatrician would normally deal with,” he said.
Dr. Pliszka approved the medications, and because the boy’s case was so difficult, obtained treatment for him at his clinic. The boy went on to do well, but without CPAN, the impact of losing his medications would have been catastrophic, Dr. Pliszka says.
“If he had gone off his medication, he would have crashed and burned, probably would have ended up in the hospital,” he said. “And then the foster parent might have said, ‘I can’t take him back,’ or ‘He’s too difficult for me.’”
That would have had ripple effects far beyond the boy and his foster family.
“A 20-minute phone call probably saved the state of Texas about half a million dollars if you added up the cost of a psychiatric hospitalization, plus a breakdown in placement, and a stay in a residential treatment center,” Dr. Pliszka said.
The Texas Legislature created CPAN in 2019 as part of a larger group of programs designed to improve psychiatric care for young people. (See “What Is the Texas Child Mental Health Care Consortium?” page 28.) Dr. Pliszka’s case highlights its primary aims
to:
- Expand primary care access to child and adolescent psychiatric consultation, training, and support;
- Manage mental health needs within primary health care settings; and
- Deliver referral and access to mental health specialty care services – aside from just telephone consultations – for patients requiring specialized treatment from a community-based mental health professional.
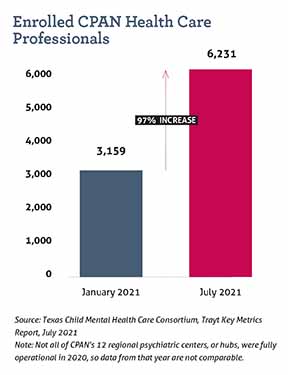
Interest in CPAN has grown steadily among physicians, and those who have used it report increased comfort with treating behavioral health, according to data compiled by the program. (See “Physician Reactions to CPAN,” page 30.)
Despite that – and despite the fact that Texas has a shortage of behavioral health professionals – many Texas physicians remain reluctant to use this service because they were not trained to handle behavioral health care, says Nhung Tran, MD, a developmental-behavioral
pediatric specialist in Austin who serves as CPAN’s pediatric consultant and the Texas Pediatric Society’s liaison to CPAN. (See “Supply and Demand,” page 32.)
More physicians need to take advantage of it, both because so many young Texans need mental health treatment and otherwise would not get it, and to help ensure that CPAN continues to receive strong support from Texas lawmakers, she says.
“We’re really taking all the practicing family care physicians and pediatricians and trying to retrofit their practices to incorporate mental health. In the past you could say, ‘I don’t know what I’m doing. Now you can’t do that anymore. … You now have
CPAN. You have a whole state of mental health people ready to [help].”
Find more information, and register, at (512) 843-3007 or by email at CPAN@austin.utexas.edu. Once registered, you can use the service by calling (888) 901-CPAN. A pediatric psychiatrist, psychologist, clinical social worker, or social service resource specialist will return your call usually within 30 minutes.
 Anxiety, depression, and more
Anxiety, depression, and more
CPAN is based on a Massachusetts model started in 2004 and now copied in 36 other states, according to Laurel L. Williams, DO, medical director for the body that coordinates CPAN’s services and a professor at Baylor College of Medicine in Houston.
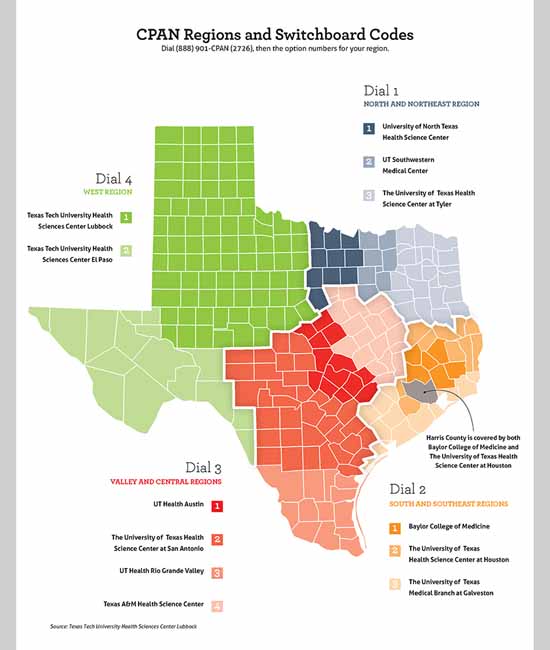
Similar to Massachusetts – but unlike some small states – Texas’ version of CPAN breaks the state into regional hubs. In each of Texas’ 12 regions, a university-based department of psychiatry provides consultation to pediatricians and family physicians
looking for answers about patients’ psychiatric symptoms. (See “CPAN Regions and Switchboard Codes,” page 27.)
CPAN opened its doors in May 2020 when many Texas primary care physicians were largely shut down because of COVID-19. That unfortunate timing led to a slower-than-expected start for CPAN. (See “Use It or Lose It,” December 2020 Texas Medicine, pages
34-37, www.texmed.org/UseCPAN.)
But by the time physicians reopened offices in the weeks that followed, they found more and more children struggling with behavioral health problems, says Dallas pediatrician Nicole Corrigan-Garrett, MD.
“One of the side effects of the pandemic has been an increased need for psychiatry and therapists as our kiddoes have had more anxiety and depression because of a battery of things happening, whether it being unable to go to school, unable to [take part
in] activities, [or] family deaths because of COVID,” she said. “The impacts have caused a domino effect.” (See “Caring for Generation COVID,” page 34.)
Many physicians call CPAN believing it is simply a referral line where they can find a psychiatrist or therapist, Dr. Pliszka says. But CPAN was set up to advise family physicians and pediatricians on the best ways to handle care for uncomplicated cases
such as anxiety or depression so that behavioral health professionals can focus on patients with more serious problems.
“Our goal is to get as much managed by the [primary care physician] as possible,” he said. “What they’ll get is help with managing the patient if they want that, and help with resources in the community.”
Austin pediatrician Wesley Glazener, MD, says he typically gets a call back from CPAN in 30 minutes from someone who can advise him.
“At any age, mental health [treatment] can be tough to sort through, and having somebody sit down and hear a story and help you decide what to do, or ‘Have you thought about this?’ or ‘I recommend that you do that’ – that’s very helpful,” he said.
CPAN also puts physicians in touch with local resources and works as a kind of triage center, identifying patients most in need of scarce psychiatric resources, Dr. Corrigan-Garrett says.
“I’ve had patients who needed intervention,” she said. “They needed intensive therapy and medication to avoid an ER situation, and CPAN definitely helps with that. And that’s not something I’ve had access to because my [psychiatric] resources were overstretched
at this point. [CPAN] has been clutch many times, and families have been very grateful.”
Some physicians hesitate to do even basic behavioral health treatment and are unlikely to ever use CPAN, Dr. Tran says. So CPAN instead has focused much of its outreach on physicians and other health care professionals who are enrolled in the program
but seldom or never use it.
“They haven’t dipped into uncomplicated anxiety and depression management cases, and we’d love them to [do that] because those are the majority of cases,” she said. “CPAN offers quite a bit, but utilization is lagging.”
Tex Med. 2021;117(11):26-30
November 2021 Texas Medicine Contents
Texas Medicine Main Page