
Vivian H. Porche, MD, has been mentoring young African American students since the 1990s, but only a handful followed in her footsteps to become a physician. One of those rare successes came last month when Victoria Beamer, MD, walked across the stage and earned her degree at Wake Forest Medical School in North Carolina.
“I met [Dr. Beamer’s] parents while I was in the line for my eldest child’s graduation” at Hampton University in Virginia, Dr. Porche said. “[Dr. Beamer] was in high school and her mother was just like, ‘Well, you seem like a nice person, would you mind if my daughter came and visited with you in her last year before she goes to college?’ And I said, ‘Oh, yes, she can even stay with me.’”
In high school and again in college, Dr. Beamer shadowed Dr. Porche, a professor of anesthesiology and perioperative medicine at The University of Texas MD Anderson Cancer Center in Houston. Dr. Porche, the first black woman to become a full professor at MD Anderson, remained her mentor through medical school.
For Dr. Porche, the payoff in Dr. Beamer’s graduation is personal – the gratification of helping a talented student into and through medical school. But it’s also professional.
“Here at MD Anderson, the patients are so diverse,” she said. “The patients come from everywhere, and I believe the patients want to see and need to see people who look like them, and I believe that helps them get better.”
Research backs up that belief. Black men historically mistrust the U.S. medical system and have the lowest life expectancy of any demographic group in the country, according to a 2018 study published by the National Bureau of Economic Research (tma.tips/NBERStudy/).
But they are more likely to select every preventive service prescribed once they meet a physician who is of the same race, the same study found.
That outreach works the other way as well. Black, Hispanic, and other minority physicians tend to set up practice in medically underserved areas and treat minority patients more frequently, according to a 2013 study in the Journal of the American Medical Association (tma.tips/JAMAMinority).
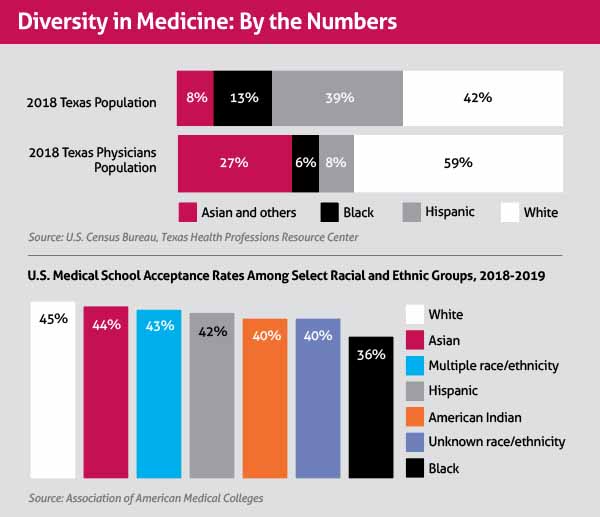
Physician diversity is widely accepted as the “key component” to delivering quality, competent care throughout the U.S., states a 2014 report by the Association of American Medical Colleges (AAMC). But Texas’ physician workforce still does not resemble the state’s diverse population. (See “Diversity in Medicine: By the Numbers,” page 40.)
That disparity reflects national trends, and there are several factors behind it, says Dale Okorodudu, MD, assistant professor of internal medicine for pulmonary and critical care at UT Southwestern Medical School in Dallas. He founded Black Men in White Coats, a group designed to provide “inspiration and mentorship” to minorities interested in medicine.
In many cases, black and Hispanic students come from homes with no college graduates and attend public schools with few resources, Dr. Okorodudu says. Many of these students also live in poverty and frequently run up against long-standing prejudices.
Such obstacles contribute to a lack of role models and mentors in medicine, as well as other fields related to science, technology, engineering, and math (STEM), he says.
Dr. Okorodudu’s group is one of several formal and informal physician networks in Texas trying to change the dynamic in medicine by providing role models and mentors for students from underrepresented groups.
But one of the biggest lessons he learned is that minority physicians cannot do that job alone.
“You don’t have to be a black male or a minority to mentor a minority student – anybody can do it,” he said. “There’s just not enough [minority physicians] to do it, so we need other people to help us do that work.”
The path to mentorship
African Americans and Hispanics are both underrepresented in medicine, but data show that African Americans face some of the biggest obstacles, namely the lowest rate of acceptance to medical schools. (See “Diversity in Medicine: By the Numbers,” above.)
Dr. Okorodudu, a mentor since 2003, launched Black Men in White Coats in response to AAMC’s research showing that between 1978 and 2011, the number of black males entering U.S. medical schools had declined as the numbers for all other demographic groups – including black females – had risen. That trend persists, according to more recent AAMC data.
One of the most surprising things Dr. Okorodudu found is that many physicians don’t feel confident about mentoring.
“With a lot of individuals, I’d say, ‘Come mentor with us.’ And one of the first things they’d say is, ‘I haven’t been a pre-med in 10 years, 15 years, 30 years. I don’t know if I still know that,’” he said.
Students should be mentored differently depending upon their age, says Eric Tait, MD, an internal medicine specialist in Houston. For instance, high school students are mainly concerned about the amount of training it takes to become a physician.
Once in college, students usually become more concerned about matters like student debt, keeping up their grade point average, and doing well on the Medical College Admission Test (MCAT), says Dr. Tait, who does presentations with Baylor College of Medicine in Houston and mentors informally. African American students often cannot afford the MCAT application fees or the expensive test prep courses many people need to get acceptable marks on the test. Dr. Tait said in his experience “that’s the number one reason that keeps most students of color out of medical school.”
STEM fields require a strong background in math and science that many African American and other minority students don’t get in often-underfunded public schools, says James Phillips, MD, professor emertius of pediatrics and former dean for diversity at Baylor. Mentors should work with students on these kinds of deficits, but it’s important to work with parents, too, when possible.
Many minority parents have not been through college themselves and don’t understand the requirements needed for a medical career path, so Dr. Phillips encourages them to get students involved in math and science programs and contests, as well as summer enrichment programs, starting in elementary school.
Lows and highs
Mentors help students at all education levels cope with the stress of being a minority in high-pressure situations. African American medical students sometimes face racial prejudice while in training, says Dr. Okorodudu. When he was in medical school, a patient suddenly became “very rude and demeaning based on my heritage,” he said.
“As a medical student, that’s hard to deal with because you’re standing there and wondering, ‘How do I respond to this patient?’” he said. “I don’t want to say anything disrespectful because I’m being graded.”
Fortunately, his attending physician intervened. However, many minority medical students don’t get that kind of support. Mentors can help them discuss the best ways to handle that kind of situation.
More often, the stress felt by minority students takes on more subtle forms, such as feeling like they always stick out in a crowd, says Shaun Smart, MD, a Houston neurologist who helps students through UTHealth and the Houston chapter of 100 Black Men, a national organization that works to improve quality of life for African Americans.
“There’s pressure and expectations that others may not feel,” he said. “When you are few in number and you make a mistake, which we all do, the issue with that mistake multiplies more in your mind and everybody else’s mind.”
Stressors like these can erode even the best student’s confidence, Dr. Okorodudu said. One of the most frequent problems he sees is talented students with “imposter syndrome,” the belief that they’re fooling others about how good they are.
He frequently has to tell these students, “‘that guy over there is not any smarter than you. He had better preparation in high school, but he’s really not smarter than you.’ Once you get them over that hump they tend to do a lot better,” Dr. Okorodudu said.
Mentors don’t just take the stress off – they also can make education fun, Dr. Smart says. When he was a high school student in Pompano Beach, Fla., the owner of a local company helped start a robotics club at his high school in a low-income black neighborhood. The club soon came in fifth place at a robotics competition that included schools from across North America.
“Help like that just changed my perspective on so many things,” he said.
Being a mentor and role model also brings its own rewards, Dr. Smart says. He does neurology presentations, and connecting with students is a great feeling.
“I’ll have a parent come up to me and say, ‘That really affected my kid,’” Dr. Smart said.
A physician of any race or gender can be a mentor or role model, says Jamboor Vishwanatha, PhD, director of the Texas Center for Health Disparities at the University of North Texas Health Science Center at Fort Worth. But people who mentor students from a different cultural background should learn as much as possible about the students they’re working with to mentor effectively.
“If you’re mentoring as if everyone is the same, I think the message gets lost,” he said.
Mostly mentoring involves showing young people what’s possible and then showing them how they can achieve it, Dr. Tait says.
“A lot of it is just laying out a vision and a pathway,” he said. “And getting them to focus on the most important things.”
SIDEBAR
TMA Diversity in Medicine Scholarships
The Texas Medical Association offers $10,000 scholarships to first-year African American, Hispanic, and Native American medical students. Acceptance for applications for the 2020-21 academic year begins Aug. 1. The Diversity in Medicine Scholarship Program is made possible with a grant from the TMA Foundation. Visit www.tmaloanfunds.com and select "Scholarships."
Tex Med. 2019;115(6):38-41
June 2019 Texas Medicine Contents
Texas Medicine Main Page