As in nearly every other sphere of modern life, technology has delivered enormous improvements in medicine. Once-unimaginable diagnostic tools and treatments are now commonplace.
Health information technology (HIT), properly implemented, has tremendous potential to advance quality of care, prevent certain types of medical errors, and streamline health care delivery. Recognizing this potential, the government and employers are pushing physicians and providers to adopt HIT quickly so they can better measure the “value” they receive for their health care dollar.
Physicians themselves, of course, are motivated to provide the best possible care, which in modern times involves the use of various technologies, including HIT. In spite of the great potential, HIT needs significant work to make it more efficient and effective for patient care. Many physicians find they are clicking more but achieving less. Currently, it’s too expensive, too disruptive to patient care, and prevents physicians and providers from sharing patient data in a timely, secure manner.
Electronic Health Records
The American Recovery and Reinvestment Act (ARRA) of 2009 allocated more than $90 million in grants to Texas to improve HIT across the state. Within ARRA is the Health Information Technology for Economic and Clinical Health Act (HITECH), which authorized incentives of up to $63,750 per physician participating in Medicare or Medicaid to adopt electronic health records (EHRs) that meet meaningful use standards. These incentives are particularly helpful, as the technology is very expensive; physicians — especially in solo and small group practices — frequently cite cost as a major barrier to EHR adoption.
In spite of the federal incentives, EHRs are still cost-prohibitive. Not all physicians are eligible for the incentives. The average EHR purchase initially costs at least $40,000 per physician, not including productivity dips that hurt practice revenues. Associated costs, such as EHR interfaces, patient portals, training, upgrades, and annual licensing fees go above the initial purchase cost and, in some cases, have not been fully anticipated. Sixty-three percent of Texas physicians whose practices are not implementing an EHR indicate it was cost-prohibitive to do so.[29]
In addition to rolling out EHR systems, physicians have had to meet nearly 100 other mandates from HITECH and the Affordable Care Act, all of which impact physicians’ practices and do little to improve care quality.
One federal requirement physicians have worked hard and in good faith to meet are the goals for “meaningful use.” The program requires physicians to use EHRs to collect and track data on 14 different measures, most of which are focused on primary care. For instance, all physicians must record and report a patient’s weight — even for specialty care where this requirement isn’t useful, such as ophthalmology.
A recent RAND study found:
- EHRs had important effects on physician professional satisfaction, both positive and negative. The current state of EHR technology significantly worsened professional satisfaction in multiple ways. Poor EHR usability, time-consuming data entry, interference with face-to-face patient care, inefficient and less fulfilling work content, inability to exchange health information between EHR products, and degradation of clinical documentation were prominent sources of professional dissatisfaction.
- Physicians approved of EHRs in concept, describing better ability to access patient information remotely as well as improvements in quality of care. Physicians, practice leaders, and other staff also noted the potential of EHRs to further improve both patient care and professional satisfaction in the future as EHR technology — especially user interfaces and health information exchange — improves.
- Excessive productivity quotas and limits on time spent with each patient are major sources of physician dissatisfaction. The cumulative pressures associated with workload were described as a “treadmill” and as being “relentless,” sentiments especially common among primary care physicians.
- Physicians describe the cumulative burden of rules and regulations as overwhelming, draining time and resources from patient care.
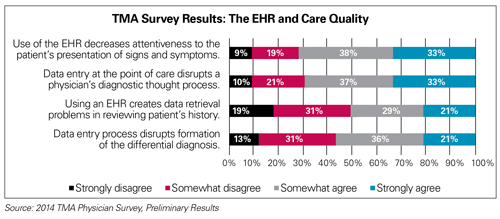
As more Texas physicians use EHRs, it is imperative that patient safety remain top of mind. Studies now indicate that using EHRs can introduce new types of errors. These errors can be caused by system use or misuse. Requiring a physician to rely on a system that is counterintuitive to his or her clinical training could result in adverse outcomes for patients. Even expert users find that EHRs require more physician time than paper records and can interrupt the patient-physician interaction in the exam room. More than 70 percent of the physicians responding to a recent TMA survey agreed that use of an EHR decreases attentiveness to the patient’s presentation of signs and symptoms.[30] Other physicians report that electronic records often lack or conceal critical information needed for patient care. Governments at all levels must carefully consider the unintended consequences that new regulations have on patient care.
Physicians who change practices or switch EHRs now find preserving the patient’s electronic health record either impossible or prohibitively expensive. TMA would like to see industry-wide changes preventing vendors from holding data hostage when physicians choose to change EHR vendors. TMA has asked the American Medical Association (AMA) to work at the federal level to achieve EHR data portability as part of the Office of the National Coordinator for HIT (ONC) standards for EHR product certification. AMA is also working to improve transparency around proprietary data storage.
In spite of the problems, 68 percent of physicians in Texas use an EHR in their practice, and this number is expected to swell to 80 percent by 2018. As EHR use continues to expand, it is critical that federal and state governments strive to protect patients and their physicians in this evolving technological environment.
We must continue working toward developing a strong HIT infrastructure in Texas that supports physician workflow while enhancing the quality and cost-effectiveness of patient care. TMA further supports strong patient privacy protections and technical standards so that patients and physicians can trust the sharing of health care information across the care continuum.
Health Information Exchange
Health information exchanges (HIEs) are supposed to help physicians and providers share patient information quickly and securely. The ability to have the right information at the right time to enhance care quality is one of the greatest promises of digitized medicine. Unfortunately, it is very difficult and costly to map patient data across disparate proprietary EHR systems. Because of the cost, HIEs are prioritizing connections with large health care institutions that have significant amounts of patient data. Unfortunately, this approach is leaving many physicians out of the communication loop, unable to share patient information securely through an HIE. Many physicians still have to share patient information via secure fax machines.
HIEs must provide complete, timely, and relevant patient information as part of the physician’s workflow, at the point of care, in a fully enabled electronic information system. Patients and their physicians must have confidence that the patient information shared is reliable, private, secure, and delivered in a manner that complies with HIPAA.
Most HIEs are in their infancy and need significant maturation before they are used ubiquitously. Until interfaces are standardized as to the minimum data set required, physicians and other health care providers should not be forced to use HIEs. Only when HIEs are well established, highly utilized, and deliver reliable patient information at a 99-percent rate of complete accuracy should they become integrated into physicians’ and providers’ practices.

- Enact legislation and rules that provide positive incentives for physicians to acquire and maintain health information technology.
- Do not penalize physicians who choose not to participate in the federal Medicare meaningful use program.
- Help physicians preserve the patient medical record in an electronic format through better data transition requirements of proprietary EHR vendors.
- Establish patient safety, privacy, and quality of care as the guiding principles for all HIE efforts. Cost reduction and health care efficiency are the expected byproducts.
- Require regulatory agencies to align physician office technology requirements so they minimize the disruption to physician workflow and patient care.
- Encourage HIE participation through legislation that will hold physicians responsible only for their own actions or inactions in regard to a possible breach of protected health information provided to an HIE (and not for the negligence or bad behavior of others).
- Eliminate the tracking of and accounting for all disclosures of patient information (when an electronic health record is used) and return to the previous mandate to track disclosures that are NOT for treatment, payment, or “health care operations.”
- Allow for the release of medical record copies in any reasonable format the health professional chooses.
- Eliminate federal mandates that compel physicians to engage in unnecessary activities and reporting.
Healthy Vision 2020